It is one of the most common dermatologic diseases affecting upto 1% of worlds population.
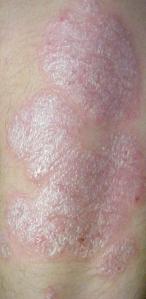
- it is chronic inflammatory skin disorder.
- in Greek it means 'to itch'
for convenience sake we divide the topic into:
- definition
- histopathology
- pathogenesis
- types
- treatment
definition:
Psoriasis is characterized by erythematous sharply demarcated papules & rounded plaques,covered by silvery micaceous scale with a predilection for the extensor surfaces,gluteal cleft,nails and scalp, a frequent positive family history, and is frequently symmetrical and usually chronic.
histopathology:

EPIDERMIS-
early changes: The first histopathological change is invasion of the epidermis by neutrophil polymorphs (and maybe a small micro abscess).
changes in established psoriasis:are essentially epidermal.
- The horny layer shows considerable hyper & parakeratosis(nuclei in stratum corneum)
- The granular layer is reduced or absent in active lesions.
- acanthosis(marked epidermal hyperplasia)
- The rete ridges are greatly elongated & often clubbed. They are separated by oedematous papillae, also club shaped
- Mitotic activity is the basal and suprabasal cells are greatly increased.
- Cellular invasion(of neutrophils) takes place, particularly in the suprapapillary region to form the Munro 'micro abscess' which are extruded in the horny layer or they may collect in disintegrated malphigian cells, the cytoplasm of which had been lysed to form the multilocular or spongiform pustule of Kogoj.{The spongiform pustule of Kogoj, one of the most characteristic features of psoriasis is located in the uppermost portion of spinous and granular layers. Here neutrophils lie intercellular in a multilocular pustule in which sponge like network is composed of degenerated and flattened keratinocytes.}
In the DERMIS the main changes consist of papillary oedema, dilatation and tortuosity of the papillary capillaries and a mild to moderate infiltrate of lymphocytes with occasional histiocytes.
pathogenesis:
- Recently, clinical studies provided fairly direct evidence for an involvement of T cells in the pathogenesis of psoriasis .T- lymphocytes release proinflammatory cytokines and lymphokines that stimulate keratinocyte proliferation and induce abnormal epidermal maturation.
- strong association with HLA-Cw*0602 allele(histocompatibility complex)
- TNF(tumor necrosis factor) is a major mediator in pathogenesis.
- A further point is that the whole skin is abnormal in psoriasis. Thus in a patient with very active disease if some of the skin that appears not to be involved with psoriasis is scratched or traumatised with a burn or cold then a psoriatic lesion might develop there. This phenomena is referred to as Koebner's phenomena. Koebner's phenomena is also seen in some other diseases like lichen planus & Vitiligo..
- A form of psoriasis, guttate psoriasis comprising small droplet like lesions all over the body, particularly common in early life, appears to follow streptococcal sore throats. Again, like the HLA evidence this all suggests some sort of prominent role for the immune system in the disease.
note:provocation factors-
Psoriasis is marked by periods of remissions and exacerbations. Remissions usually last a few weeks to many years. Both local and systemic provocation factors bring in exacerbations.
- Local Factors: Local injury to the skin produces psoriatic lesions, the well-known Koebner Phenomenon.
- Trauma involving the papillary dermis could be physical, chemical, mechanical, allergic or burns, drug eruptions, dermatitis, lichen planus, miliaria, herpes zoster, chickenpox etc. Koebner phenomenon occurs usually within 7-14 days (ranging from 3 days to 3 weeks)
- Seasonal variations: In most patients, psoriasis worsens during cold weather. High humidity is usually beneficial, whereas sunlight worsens in some but improves in many.
- Pregnancy:In most cases pregnancy induces remissions, though raised levels of progesterone in the latter half of pregnancy can precipitate generalized pustular psoriasis in some.
- Emotional Stress: Psoriasis is well known to be induced, exacerbated, or sustained due to emotional stress. The mechanism is not yet well understood, but neuropsychoimmunological mechanisms are hypothesized. The disease itself could produce a reactive depression, which could further exacerbate the disease.
- Infections:Streptococcal URTI has been shown to exacerbate existing psoriasis and precipitate an attack of acute guttate psoriasis mainly in children.
- Drugs:Many drugs are known to precipitate or exacerbate psoriasis.
- Beta-blockers like propranalol, practalol, and metapralol may induce or exacerbate psoriatic eruption.The eruption usually disappears within 2 to 6 weeks of cessation of the drugs.
- Almost all NSAIDS affect psoriasis adversely.
- Anti depressants like lithium compounds and Trazodone may precipitate generalized pustular psoriasis.
- Too rapid withdrawal of corticosteroid therapy may precipitate pustular or erythrodermic exacerbations of psoriasis.
- Alcoholic beverages affect psoriasis adversely.
- Chloroquine, clonidine, iodides, glibenclamide, and tetracycline are a few other drugs known to exacerbate psoriasis.
types:
Plaque psoriasis(psoriasis vulgaris)is characterized by raised inflamed lesions covered with a silvery white scale. The scale may be scraped away to reveal inflamed skin beneath. This is most common on the extensor surfaces of the knees, elbows, scalp, and trunk.

Guttate(drop shape) psoriasis presents as small red dots of psoriasis that usually appear on the trunk, arms, and legs; the lesions may have some scale. It frequently appears suddenly after an upper respiratory infection (URI).

Inverse psoriasis occurs on the flexural surfaces, armpit, groin, under the breast, and in the skin folds and is characterized by smooth, inflamed lesions without scaling.

Pustular psoriasis presents as sterile pustules appearing on the hands and feet or, at times, diffusely, and may cycle through erythema, pustules, and scaling. can be localised (on palms & soles) or generalized(characterized by fever, leukocytosis, arthralgia,diffuse cutaneous & mucous pustules,secondary infection ,electrolyte disturbances)

Erythrodermic psoriasis presents as generalized erythema(more than 90% skin), pain, itching, and fine scaling.

Scalp psoriasis affects approximately 50% of patients, presenting as erythematous raised plaques with silvery white scales on the scalp.
Nail psoriasis may cause pits on the nails, which may develop yellowish color(resembles oil drop under nail plate) and become thickened. Nails may separate from the nail bed.


Psoriatic arthritis affects approximately 10% of those with skin symptoms. it is asymmetric inflammatory arthritis most commonly affecting distal & proximal interphalangeal joints.
Oral psoriasis may present with whitish lesions on the oral mucosa, which may appear to change in severity from day to day. It may also present as severe cheilosis with extension onto the surrounding skin, crossing the vermillion border.
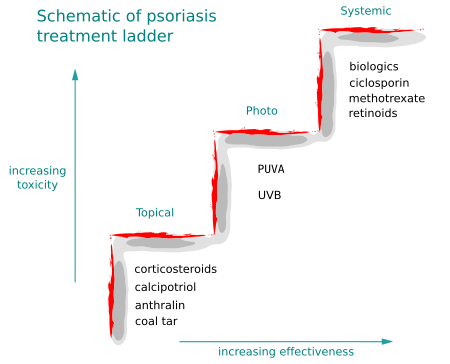
topicals:
Topical steroids:
- Topical steroids are the most widely used medications for psoriasis. They are effective, convenient to use and affordable.
- Most common side effect is cutaneous atrophy. But the atrophy is reversible in most cases if medication is discontinued early. Other side effects are telangiectasia, folliculitis, perioral dermatitis etc.
- Many dermatologists believe that tachyphylaxis and steroid rebound are major limitations of long-term therapy with steroids in psoriasis.
- Treats inflammatory dermatosis responsive to steroids. Decreases inflammation by suppressing migration of polymorphonuclear leukocytes and reversing capillary permeability.
- Triamcinolone acetonide -Has mild potency and is the first DOC for most patients.
- Betamethasone dipropionate -Is a potent topical steroid and is DOC if psoriasis is resistant to milder forms.
- oral steroids should not be used for psoriasis since risk of developing pustular psoriasis if therapy discontinued.
Coal tar
- An inexpensive treatment that is available over the counter in shampoos or lotions for use in widespread areas of involvement. It is particularly useful in hair-bearing areas.
- Antipruritic and antibacterial that inhibits deregulated epidermal proliferation and dermal infiltration. Does not injure the normal skin when applied widely and enhances the usefulness of phototherapy. Generally is used as a second-line drug therapy due to messy application, except for shampoos, which may be used and rinsed at once.
- Goeckerman regimen. Once or twice daily, crude coal tar is applied and then removed before the patient is exposed to total body UVB light. This is followed by a cleansing bath or shower to remove the residual tar and scales.
- Adverse reactions:
- Staining and odour of the tar, lessened in newer preparations
- Folliculitis (Commonest)
- Primary irritant reaction if used in areas like face, genitalia and flexures.
- Carcinogenecity: In cases of prolonged usage with UV light therapy.
Contraindications:
1. Erythrodermic Psoriasis
2. Generalized Pustular Psoriasis
3. Pre-existing folliculitis/ severe acne
Dithranol/Anthralin:
- It is a synthetic derivative of chrysarobin, a tree bark extract. Since it is an unstable product, combining with salicylic acid stabilizes it.
- adverse:highly irritant especially on the head and neck areas and stains linen irreversibly.
- The Ingram regimen
The Ingram regimen combines anthralin paste, a coal tar bath and UV exposure. Anthralin is applied to lesions as a thick paste. Once the anthralin is removed, the patient is then exposed to UV and may also take coal tar baths. Generally, a patient using the Ingram regimen in the hospital or day treatment program will require three weeks of therapy, clearing in an average of 20 days.
Vitamin D-3 analog (calcipotriol)
- Used in patients with lesions resistant to older therapy or with lesions on the face or exposed areas where thinning of the skin would pose cosmetic problems.
- Mechanism of action is through induction of terminal differentiation of keratinocytes and inhibition of T cell proliferation.
- It is widely used in chronic plaque psoriasis alone or in combination with potent steroid
- The lesions and surrounding uninvolved skin may be irritated following treatment; if this happens, discontinue treatment; it may transiently but reversibly elevate serum calcium; discontinue if increase is outside the normal range
retinoid (tazarotene)-
- A retinoid prodrug that is converted to its active form in the body and modulates differentiation and proliferation of epithelial tissue and perhaps has anti-inflammatory and immunomodulatory activities. May be the DOC for those with facial lesions who are not at risk of pregnancy.
- adverse:
- May cause a feeling of burning or stinging
- caution patients to take protective measures against exposure to ultraviolet or sunlight, since photosensitivity may result
phototherapy:
There are two main forms of phototherapy, that based on ultraviolet B therapy, most commonly given as narrowband or TLO1 therapy, and PUVA therapy. PUVA stands for psoralen + UVA.
PUVA-
- It consists of ingestion of Psoralen in the dose of 0.6-mg/kg body weight on alternate days and followed in 2-3 hours later by UV radiation for graded periods.
- The commonly used psoralens are 8-methoxy psoralen and 4,5,8 trimethoxy psoralen.
- PUVA therapy affects DNA synthesis and proliferation of cells in psoriatics by 2 mechanisms:
- An anoxic reaction that affects cellular DNA with the formation of photo adducts.
- An oxygen dependent reaction where free radicals and reactive oxygen formed may damage the membrane of lipid per oxidation and induce activation of mediators of the eicosanoid system.
- PUVA therapy also reduces the chemo tactic activity of the psoriatic leukotactic factor.
- Topical PUVA has been tried in the form of PUVA bath. Trimethoxy psoralen 50mg in 100ml ethanol is added to a 150-litre bath. Patient is allowed to bath for 15 minutes and then exposed to UVA at 290-320 nm. Photosensitivity is achieved immediately after this bath is 15 times greater than after oral psoralen and side effects like nausea, headache can be minimized by PUVA bath.
- Side effects of PUVA therapy:
- Nausea, vomiting, headache, vertigo, erythema, pruritus, blistering
- Koebner phenomenon
- Hypertrichosis, hyper pigmentation
- Lichenoid eruption
- Photo-onycholysis
- Premature ageing of skin, Cataract formation
- Increased incidence of skin cancers etc.
Ultraviolet B
The main wavelength in natural light that appears to be effective is ultraviolet B (despite most natural light being UVA). Experiments have shown that particular wavelengths of ultraviolet radiation between 310 to 315 nanometers. A particular lamp has been developed with a peak exposure within this area (so called narrowband or TLO1 lamp) and this is highly effective for psoriasis. It is however not as effective as PUVA treatment but is administered similarly on a twice weekly basis. In general most patients would be treated with TLO1 first and if this failed or the remission induced was not good they would be treated with PUVA on the following occasion
note:UV therapy is contraindicated in patients taking cyclosporine & used with care in immunocompromised since increased risk of developing skin cancers.
Systemic Treatments
In general the rule is start with topical agents, move onto phototherapy and if this fails consider systemic agents.
this includes biologics(targeted drugs) & 3 other drugs-
methotrexate:
Methotrexate -antimetabolite.It acts on 's' phase of cell cycle
Contraindications:
- Absolute: Pregnancy, Lactation
- Relative: Decreased renal function, hepatic disease, severe hematological abnormalities, alcoholism, child bearing age (12weeks before conception: should be stopped in both sexes), active infectious diseases, h/o potentially serious infection that could be reactivated, immunodeficiency syndromes, unreliable patient.
- Oral dose: single, or more commonly 3 divided doses at 8 am, 8 pm, 8 am once a week (Rationale: Presumed cell kinetics in psoriasis cell cycle shortened from 19 days in normal to 37.5 hours in psoriatic epidermis.) i.e,3 doses taken for 2 days.remaining 5 days folic acid is taken(to prevent toxicity to normal body cells)
- Initial dose-5-10 mg stat: CBC(complete blood count), LFT(liver function tests) after 7 days.
- If Okay, escalate dose to 2.5-5mg per week to get reasonable benefit without toxicity.
- 10-12.5 mg/week on an average gives maximum benefit.
Adverse Effects:
- Hepatotoxicity: Regular monitoring to detect
- Pulmonary Toxicity: Pneumonitis, Pulmonary Fibrosis
- Hematological Effects: Myelosupression
- Gastrointestinal: Nausea, diarrhoea, ulcerative stomatitis, anorexia, vomiting
- Potent Teratogen
- Other: alopecia, fatigue, phototoxicity, headache, and dizziness.
Retinoids are synthetic or natural analogues of vitamin A.
The 3 main ones are:
1. Isotretinoin (13 cis retinoic acid)
2. Etretinate
3. Acitretin
Acitretin is an active metabolite of Etretinate. Etretinate is an ester and acitretin a corresponding free acid. Its great advantage over etretinate is its decreased lipophilicity, which results in elimination half-life of 50 hours as opposed to more than 80 days for etretinate. However the clinical efficacy and side effects are similar to etretinate.
The mode of action of retinoids is not fully established. It seems to induce a better maturation in keratinocytes and to reduce the neutrophil chemotaxis in pustular psoriasis.
Indications:
- 1. Generalized Pustular Psoriasis: Considered to be the drug of choice.
- 2. Psoriatic erythroderma.
- 3.Severe psoriasis vulgaris, where other modalities have either failed or are contraindicated.
- 4.Palmo-plantar pustular psoriasis.
Dose:
0.5-1 mg/kg/day is the usual initial dose of etretinate. Maintenance dose of 0.5 to 0.75mg/kg/day. Remission may take anywhere from 12-24 weeks. Relapses are very common following discontinuation of treatment.
Acitretin- an optimum dose of 50mg daily (mean 0.66mg/kg/day) is recommended.
Contraindications:
1.Women of child bearing age, unless the psoriasis is unresponsive to other therapies or where clinical condition contraindicates the use of other regimens.
In such cases the following precautions are to be strictly adhered to:
a. Has received both oral and written warning of hazards of taking acitretin
b. Should be on reliable form of contraception
c. Should have negative serum and urine pregnancy test done at least 1 week prior to beginning treatment.
d. Treatment should be started on the 2nd or 3rd day of next normal menstrual period.
2. Pregnancy
3. Children
4. Active liver disease
5. Pre-existing hyperlipidemia
Side Effects:
Almost 99% of patients receiving retinoids develop some sort of side effect.
- It is highly teratogenic.
- The retinoids are lipophilic and are retained in the body for a considerably longer period of time. So women receiving the drug should avoid pregnancy for a period of 3 years.
- Lipid abnormalities in the form of increased serum triglycerides and cholesterol may necessitate discontinuation of therapy. In mild cases, the abnormality may be alleviated by concomitant administration of fish oils.
- Liver enzyme elevation, hepatitis and jaundice
- Radiological spinal changes including anterior spinal ligament calcification, osteophytes, disc abnormality, DISH (diffuse idiopathic skeletal hyperosteosis) can occur
- In children, premature closure of epiphyses, growth retardation and hyperosteosis can occur
- Dryness of the lip, nose, mouth, eyes, throat with peeling of skin, exfoliative cheilitis, uveitis, balanitis, gingivitis, corneal ulceration, burning sensation of skin, atrophy of skin, alopecia, epistaxis, increased bruising, generalized erythema
- Purulent paronychia may necessitate stopping of therapy.
- Pseudotumour cerebri is not uncommon
Drug Interactions:
- Do not give tetracyclines along with retinoids (pseudotumour cerebri)
- No supplementation with vitamin A
- Concommitant methotrexate increases hepatotoxicity
- Ethanol should not be given along with acitretin because it is converted to etretinate
Cyclosporine:calcineurin inhibitor
It is indicated for the treatment of adult non immuno-compromised patients with severe recalcitrant psoriasis who have failed to respond to at least one systemic therapy or in patients for whom other systemic therapies are contraindicated or cannot be tolerated.
adverse effects-
renal dysfunction, hypertension, hyperkalemia, hyperuricemia, hypomagnesemia,hyperlipidemia,increased risk of malignancy.
biologics:
| drug | mechanism | route | adverse effects |
| alefacept | anti-CD2 | IM | lymphopenia |
| etanercept | anti-TNFalfa | SC | neurologic events |
| efalizumab | anti-CD11a | SC | thrombocytopenia,hemolytic anemia |
| adalimumab | anti-TNFalfa | SC | hypersensitivity reactions,neurologic events |
| infliximab | anti-TNFalfa | IV | hepatotoxixity,neurologic events,hypersensitivity reactions, |
note:
- adverse effects shared by all biologics-potential for increased malignancies,serious infections.
- adverse effects shared by all anti-TNFalfa agents are-may worsen congestive heart failure.
- Up to 20% of patients with psoriasis have extensive skin disease, and etanercept may be the biological agent of choice for these patients.
in pregnancy:
Topical corticosteroids, calcipotriol, broad band UVB used.
- Topical corticosteroids have been widely used during pregnancy, although intrauterine growth retardation was reported in an infant whose mother applied 40mg/day of topical triamcinolone beginning at 12 weeks of gestation.
- Calcipotriene is approximately 6% absorbed when the ointment form is applied to psoriatic plaques and is likely safe in pregnancy for the treatment of localized psoriasis
- Broadband ultraviolet B phototherapy is considered the safest therapy for extensive psoriasis during pregnancy, although overheating during treatment should be avoided.
- PUVA is a potential teratogen because it is known to be mutagenic and to induce sister chromatid exchanges. However, adverse outcomes have not been reported in studies of women exposed to PUVA during pregnancy.
- Methotrexate and acitretin are both in pregnancy category X. Methotrexate can be used in women with childbearing potential who are using effective contraception. Pregnancy should be avoided for at least one ovulatory cycle after this medication is discontinued. Acitretin should not be prescribed for women of childbearing potential.
- There are limited data on the safety of biologics used for the treatment of psoriasis during pregnancy
59 comments:
Thanks for this great article…
Dear Admin,
I browse your website, its very impressive, I love that.
Psoriasis is a abhorrent disease.
Psoriasis can accomplish activity afflicted and abhorrent man. This ache is actual difficult to treat. There are abounding ointments, tablets, and procedures that are acclimated to amusement eczema. But I could not advice amusement eczema. Because of this disease, I was a hermit, did not leave the abode for 2-3 months. My wife accurate me. But one day I begin a abundant website that helped me with my problem. I acclaim that you apprehend the advice on this site
Psoriasis treatments
Best Regards
wow really superb you had posted one nice information through this. Definitely it will be useful for many people. So please keep update like this.
Psoriasis Treatment | Vitiligo Treatment
I have gone through your blog. The information you have given are really informative.Keep sharing like this info!!! its really effective!!!!
acne/pimple cure in Madurai
your blog is so inspiring. thanks for the post.
dermatologist in Bangalore
Wow such an informative blog. Got to know a lot. Thank you blogspot for such a wondreful blog. Definitely am gonna use Psoriasis medicine for this treatment.
Very informative blog. There are many Psoriasis medicines are available which help to cure from Psoriasis but the difficult thing is to choose best one. Here you can get the best knowledge regarding the medicines.
Thanks for sharing!
good blog keep posting
skin doctor in Bangalore
Last year I began using the dermalmd psoriasis serum and it’s the gift that keeps on giving…my sister and I both have psoriasis and are so pleased with how this serum helps
having psoriasis for 8 years now I started with the Dermalmd serum and been using it since..it’s not expensive and it lasts for a long time with constant results
My Psoriasis worsen in summer so I apply the Dermalmd serum as treatment and use breast milk if I have a source, lol …try both for best effect
I have psoriasis since i was 17 and i started useing the dermalmd cream for treatment.. great on the skin no irrtations and gives quick results
It's only been a month of using my dermalmd psoriasis treatment but i notice less irritatiom outbreaks and itching..overall a product worth trying
Nice observation and good article,thankyoU for sharing your knowledge,keep posting such information that's helpful to others
psoriasis cure treatment in hyderabad
Psoriasis treatment in Hyderabad
Best Psoriasis Treatment in Hyderabad
Best Dermatologist Doctors in Hyderabad
What is Psoriasis?
Psoriasis is an immune mediated inflammatory disorder of skin. It comes with raised, red and scaly patches typically on the back of elbow, front of lower leg, scalp and back.
Psoriasis Causes are not known yet but immune system and genetics play a major role as trigger factors. The skin cells of affected area proliferate at an abnormally fast rate.
Psoriasis causes are not fully understood, but scientists believe psoriasis is the result of several factors, including genetics, environmental factors, and the immune system.
Psoriasis is a chronic skin condition caused by an overactive immune system. Symptoms include flaking, inflammation, and thick, white, silvery, or red patches of skin. Psoriasis treatments include steroid creams, occlusion, light therapy and oral medications.
https://www.jrkresearch.com/psoriasis-medicines.php#happens
Hi, Great.. Tutorial is just awesome..It is really helpful for a newbie like me.. I am a regular follower of your blog. Really very informative post you shared here. Kindly keep blogging.
Psoriasis treatment in Hyderabad
Best Psoriasis treatment in Hyderabad
Top Psoriasis treatment in Hyderabad
Best skincare treatment in Hyderabad
Really Helpful Blog That's Obviously Help For psoriasis Injured People.Here we get Something New Details about psoriasis treatment.Thanks For Putting this Cool Post!!!!!!!
Psoriasis is a skin disorder that causes skin cells to multiply up to 10 times faster than normal. This makes the skin build up into bumpy red patches covered with white scales. They can grow anywhere, but most appear on the scalp, elbows, knees, and lower back. ... Psoriasis usually appears in early adulthood.But with Agbara Herbal soap and the cream, Use them together within 2weeks and everything about Your skin will be cleared , Buy this AGBARA HERBAL NATURAL SAOP AND CREAM from any Herbal store in Your Country Or You Visit drcureherbalhome@gmail.com, for you fast cure.
The information you've shared in this blog is highly remarkable. Thanks for sharing such quality information
scapho 150mg,scapho 150mg injection
I found these top hair transplant surgeons in india on the internet
Psoriasis is an auto-immune disorder characterized by excessive white flake on the scalp with itching, scratching, pain, burning slowly it covers the whole scalp, generally, it starts from folds of the body like the nape of the neck and back of the ear. It is curable and we do psoriasis treatment in easy and affordable sessions.
It's really most important article, for more visit Chlorpheniramine Maleate Syrup Suppliers in India.
Contact Dr. Deepak Bhalla for Ayurvedic Treatment for Psoriasis. Herbal medicine for Psoriasis without any side affects. Please call +91 9810584818
Thankss for sharing for more Tend Skin The Skin Care Solution Reviews
Great Blog, Buy Ayurvedic Soaps Online (Aloevera Cow Ghee Soap) at Andariki Ayurvedam Online Store.This soap is made from the finest quality of Vegetable oils and Aloe Vera. And more information we want to visit our site Buy Ayurvedic Soaps Online.
nice blog shared, great knowledge
allergy doctor
How can I explain this to the world that there is a man who can cure HERPES, I was diagnosed for the past 1 year I have being into HERPES since 1 year, so I decide to look for help in the internet then I found a post write about this great man called DR. Yakubu , people say good thing about him that this man have cured, a lot of people in the internet, him has power's to cure HSV1 AND HSV2 I don’t believe that there is a cure for Herpes Simplex Virus because though there is no cure for herpes that what I have in mind HERPES had no cure well , my HERPES is negative through the using of herbal cured of DR yakubu , I contacted this man for help because of what i see in the internet. if you need his cured just email him now on dr.yakubuherbalhealingclinic@gmail.com , thank you DR. i will never stop shearing you testimony DR. Yakubu . him Can as well CURE THE FOLLOWING DISEASE:-1, HIV/AIDS, 2, Diseases of the hear 3, Malignant tumors 4. Cardiovascular diseases 5. Diabetes mellifluous 6.Influenza and pneumonia 7.Alzheimer's disease 8. hsv1 - hsv2. If you need LOVE SPELL. E.T.C contact him dr.yakubuherbalhealingclinic@gmail.com or you whatsapp him on +2348057353647...
Dr.yakubu 하나님은 내 삶을 회복시켜 주신 것에 대한 축복을 계속할 것입니다. 나는 사람들에게 증거를 계속 나눌 것입니다.
Hi I am Dr Deepak Bhalla and I am a Ayurvedacharya I have cure for the dangerous disease Psoriasis. I have cured millions of patients in India.
I want to write about the skin disease Psoriasis. This skin disease is spread all across the world. In India Psoriasis is spread vastly in the rural as well as in urban areas. Psoriasis is a challenging papulosquamous dermatological disease with no known etiology and no perfect therapy for controlling the disease. Multiple therapies involving steroids and critical drugs like methotrexate (double edged knife drug) Are being used with unpredictable therapeutic response. Further there is no advanced clinical method to understand and evaluate the efficacy of treatment. Psoriasis is chronic relapsing disease of the skin characterized by variable clinical features. It is a challenging disorder with no known etiology and no perfect medicine for controlling the disorder. Medical professionals all over the world are looking for a safer drug which can control the Psoriasis though not cure.
The cutaneous lesions are usually so district that a clinical diagnosis is easy to make. The lesions are classified as erythrosquamous, which indicated that both the vasculature (erythema) as well as the epidermis (Increased scale formation) are involved.
The morphology of the skin lesions varies considerably. The terms commonly used to describe the different morphologic types of the disease. Psoriasis vulgaris is the most common type of psoriasis. Circular plaques are predominant on the elbows, knees, lower back, and the retroauricular areas of the scalp, whereas eruptive (guttate) lesions are often confined to the trunk and proximal extremities. Psoriatic erythroderma involves the entire body, presenting with generalized erythema and varying degrees of scale.
Psoriasis may also present in a pustular form. There is a generalized form, usually referred to as pustular psoriasis (von Zumbusch), and a localized variant, confined to the palms and soles, known as pustulosis palmaris. In rare instances, in psoriasis of the plaque type or guttate psoriasis, pustules may develop after acute relapses (psoriasis with pustules).
The clinical presentation varies depending on a number of factors, which may cause an individual to present with a few localized psoriatic plaques or with generalized skin involvement and the development of pustules. The disease activity is reflected predominantly as scaling in stationary plaques and as inflammation in the eruptive guttate lesions.
Psoriasis can be diabling not only because of skin involvement but also because of concomitant joint disease. Psoriasis arthropathy is the only recognized noncutaneous manifestation of the disease. Psoriasis can be controlled and cured completely with the help of only ayurveda. Ayurvedic medicines proved to be the best medicine for Psoriasis which can not only control from aggravating but it can also control this disease completely from the roots.
Dr. Deepak Bhalla is one Ayurvedacharya who came with success for lakhs of Psoriasis suffers all across the country. He not only cured these patients but also gave them complete relief from this disease off all age group without any side effects. Today he challenges the alopathic medicines and steroids which was given to psoriasis patients all across the world and result in death. Aurvedic medicine is miracle for this dangerous disease called Psoriasis.
Contact Detail
Dr Deepak Bhalla : +919810584818
nice information for skin
Allergy Hospital
I'm 61 years old, I contracted hpv in 2011' I has be taking lot treatment for it and embarrassed some months ago the wart stated coming out seriously, I used lot recommendation because there was lot warts around my anus and was so . but today I'm totally happy I got the virus eliminated by using natural treatment from Dr Onokun herbal center after his treatment I got cured. all the warts went away' seriously believed Dr Onokun he have the cure for human papillomavirus because he has eliminated hpv been in my body since 2011, Dr Onokun make it possible for me. Here is Dr Onokun email: dronokunherbalcure@gmail.com
Nice blog. Thoroughly loved reading it. Similarly amazed on reading the reviews of a product Psorolin medicated bathing bar - Mild and gentle bathing bar for psoriasis and dry skin removes excess skin cells and brings out your natural glow. If you wanna give your skin a dose of hydration and skin-repairing ingredients check this out Psorolin medicated bathing bar
Psoriasis is a chronic immune-mediated skin disease characterized by red, dry, scaly patches, and it can affect the body areas like the scalp, hands, elbows, back, knees, and many more. Psoriasis is not only a skin problem, but it can also affect different organs of the body, such as joints, musculoskeletal structures, nails, and eyes. Genetic predisposition is considered one of the major factor to cause psoriasis; other factors like alcohol, smoking, stress, heart problems, hypertension, obesity can also trigger psoriasis in many people. At Dr. Nivedita Dadu’s Dermatology Clinic, the best psoriasis doctor in Delhi provides various effective psoriasis treatment like oral medications, topical medications, phototherapy, excimer laser, injectable biological that helps people to manage and treat this disease effectively. These treatments assist in reducing cell proliferation rate and suppress skin irritation and reduce the symptom of psoriasis. Dr. Nivedita Dadu, psoriasis specialist doctor in Delhi also recommends some lifestyle and dietary changes that also helps to minimize the redness and irritation caused by psoriasis and help in improving this skin condition. To get the best psoriasis treatment in Delhi visit at Dr. Nivedita Dadu's Dermatology Clinic, to treat this skin condition effectively.
Disclaimer: Images and contents used in this post are only for promotional purposes.
Safe 24 Call Drivers In Madurai Acting Driver Madurai 104444it https://123just.com/ad/66/safe-24-call-drivers-in-madurai
Your blog is awesome. Thanks for sharing for such a quality information. Psoriasis Treatment London
I started on COPD Herbal treatment from Ultimate Health Home, the treatment worked incredibly for my lungs condition. I used the herbal treatment for almost 4 months, it reversed my COPD. My severe shortness of breath, dry cough, chest tightness gradually disappeared. Reach Ultimate Health Home via their website www.ultimatelifeclinic.com . I can breath much better and It feels comfortable!
Great post. Very informative & helpful for me. Keep sharing! Psoriasis Treatment London
I am very happy to see this post because it really a nice post. Thanks
Nice post. Really appreciated your intelligence. Thanks for sharing for such a wonderful blog! Psoriasis Treatment London
Hi there,
Thank you so much for the post you do and also I like your post, Are you looking for Buy Misoprostol Online in UAE? We Buy Misoprostol Online, Misoprostol in Dubai pharmacy, Abortion pills for sale in Dubai, Where i can buy abortion pills in Abu Dhabi, Abortion pills price in Dubai, Abortion pills for sale in Ajman, Where i can buy abortion pills in Dubai, Where i can buy abortion pills in Sharjah, Buy Mifepristone and misoprostol online UAE, Abortion pills cytotec available in Dubai, Buy abortion pills in Dubai, Cytotec pills in Dubai, Cytotec price in Dubai, Cytotec pills in Dubai, Cytotec price in Dubai, Abortion pills in Dubai, mifegest kit in UAE, Pregnancy termination pills in Qatar, Abortion in Dubai, pregnancy abortion pills in UAE, Mifepristone and misoprostol available in UAE, Cytotec medicine in UAE, How to get abortion pills in UAE, Abortion pills available in Dubai, Where to buy cytotec in Dubai, Abortion pills in Qatar pharmacy, Dubai online shopping tablets, Abortion clinics in muscat, Where to buy abortion pills in Bahrain, Abortion pills in Ajman, Mifegest kit price online order, Vimax pills in Abu Dhabi, Where can i buy mifepristone and misoprostol in Dubai, Can you take birth control pills in Dubai, Abortion pills in UAE for sale for you with the well price and our services are very fast.
Click here for href="https://onlineplanpharmacist.com/product/flurazepam/"/> title"flurazepam - Online Plan Pharmacist|Buy Abortion Pills Online| Buy Termination Pills in Dubai| Online Pharmacy near You"/>MORE DETAILS......
Contact Us: +1 (443) 718-9645
Email Us At: support@healthsbiopharma.com
Hi there,
Thank you so much for the post you do and also I like your post, Are you looking for Buy Sleeping Pills Online in the whole UAE? We are providing Abortion Pills in Qatar, Where I can Buy Abortion Pills in Qatar, Abortion Pills For Sale in Riyadh, Ru 486 Cytotec in Riyadh, Buy Abortion Kit Online in Riyadh ,Buy Abortion Kit Online 2021 in Riyadh, Buy Abortion Kit Online in Qatar, Cytotec 200 Mcg kikolo Online, Abortion Pills For Sale in Bahrain, Ru 486 Cytotec in Bahrain, Buy, Abortion Kit Online in Bahrain, Abortion Pills in Bahrain, Cytotec 200 Mcg in Bahrain, Abortion Pills For Sale in Jeddah, Ru 486 Cytotec in Jeddah, Buy Abortion Kit Online in Jeddah City, Ru 486 Cytotec in Riffa, Where I Can Buy Abortion Pills In RIffa, Buy Abortion Kit Online In RIffa, Abortion Pills in Dubai, Cytotec 200 Mcg in Riffa,Cytotec 200 Mcg in ,Misoprostol in Dubai pharmacy, Abortion pills for sale in Dubai, Where I can buy Abortion pills in Dubai, Abortion Pills price in Dubai, Abortion Pills in UAE for sale, Abortion pills for sale in Ajman, Where I can buy Abortion pills in Sharjah, Buy Miferpristone and Misoprostel online UAE, Cytotec price in Dubai, Abortion pills Cytotec available in Dubai, Buy Abortion pills in Dubai, Cytotec price in Dubai, Abortion pills in Dubai, Mifegest kit in UAE with the well price and our services are very fast.
Click here for title="flurazepam-Online Plan Pharmacist"/>MORE DETAILS......
CONTACT US
Phone :+1 (443) 718-9645
Email: support@healthsbiopharma.com
Wow Amazing post. Very Helpful, Thanks for sharing.
I have written a Blog about Psoriasis
https://www.sriramakrishnahospital.com/if-psoriasis-is-not-treated-what-will-happen/
Great blog on healthcare. I have read your blog and you explain everything so properly. Thanks for sharing such information.
http://skindiseasehospital.org/know-about-psoriasis/
Thank you for sharing this blog. Necessary first aid should be given as soon as the injury occurs. The first aid that can do so is to use it greatly to heal our wound quickly. Use synerheal collagen sponge dressing to cure your wounds fast and safe.
Thank you for giving this article. Injury and ulcers in the body can have very bad effects on our body if not properly maintained. I'm sure aquacel ag extra hydrofiber dressing a pioneer in wound healing.
Thank you for the article. We are primarily involved in providing the medicines you need to heal your wounds.
seeskin plus collagen sponge dressing
Nice and informative...Keep it up...Keep posting.I have also written on How vitiligo can be treated
Thanks for sharing. This post really help me a lot and I have learnt some new things from your blog,Nice post! Thank you for sharing this post with us
Regards,
Medical Skin Treatment in Manchester
Very useful Information. Kalpana Naturals Provides one of the best product to increase our Immunity.
Buy our Best product
pain relief oil by Kalpana Naturals.
Very useful Information. Kalpana Naturals Provides one of the best product to increase our Immunity.
Buy our Best product Herbal Immunity Booster by Kalpana Naturals.
Very best blog thanks for sharing keep posting.
Visit Vashikaran Astrologer in Jayanagar
Thank You for sharing this use full article. FIX GIDE GTR COLLAGEN MEMBRANE a resorbable collagen membrane has a unique bilayer structure that offers superior tissue compatibility and prevents the ingrowth of soft tissue into the augmented site.
Great posting! Thanks for sharing.
The under-eye skin is where oxygenated blood pools, causing the blue circles to appear. Blood can be seen through the thin skin on this area. However, brown or black dark rings are more typical. They develop as a result of skin surrounding the eyes being hyperpigmented.
Click here Under eye dark circles Treatment in East Delhi
for more.
I was diagnosed with Bronchiectasis four years ago. For over two years, I relied on prescription medications and therapies, but unfortunately, the symptoms continued to worsen. My breathing became more laboured, and I experienced increasing fatigue and shortness of breath with even minimal activity. Last year, out of desperation and hope, I decided to try an herbal treatment program from NaturePath Herbal Clinic. Honestly, I was skeptical at first, but within a few months of starting the treatment, I began to notice real changes. My breathing became easier, the tightness in my chest eased, and I felt more energetic and capable in my daily life. Incredibly, I also regained much of my stamina and confidence. It’s been a life-changing experience I feel more like myself again, better than I’ve felt in years. If you or a loved one is struggling with Bronchiectasis, I truly recommend looking into their natural approach. You can visit their website at www.naturepathherbalclinic.com
info@naturepathherbalclinic.com
Looking for natural hair restoration? At Looks Hair and Skin Clinic, our skilled hair transplant surgeons in Bangalore deliver natural-looking, long-lasting results using advanced FUE and FUT techniques. We focus on precision, safety, and personalized care to give you a fuller, natural hairline. Restore your confidence with expert treatment at Looks Hair and Skin Clinic today.
Klick Digitally is one of the best digital marketing agency for hair transplant clinics, offering specialized strategies that deliver real growth. With deep expertise in the hair restoration industry, Klick Digitally helps clinics attract high-quality leads through SEO, Google Ads, social media marketing, and GMB optimization. Their targeted campaigns focus on patient intent, local search visibility, and brand credibility, ensuring maximum ROI. Whether you want more consultations, stronger branding, or consistent inquiry flow, Klick Digitally provides tailored solutions that truly work. Choose Klick Digitally to elevate your clinic’s online presence and achieve sustainable patient growth.
Psoriasis laser treatment Langley
Psoriasis laser treatment in Surrey
Post a Comment