Based on aetiology:
infective type:
- Bacterial
- localised otitis externa(furuncle)
- diffuse otitis externa
- malignant otitis externa
- Fungal
- otomycisis(fungal otitis externa)
- viral
- herpes zoster oticus
- otitis externa haemorrhagica
reactive type:
- eczematous otitis externa
- seborrhoeic otitis externa
- neurodermatitis
furuncle:
Aetiology-staphylococcal infection of hair follicle
clinical features-
- severe pain & tenderness which are out of proportion to size of furuncle
- movements of pinna painful
- jaw movements painful
- if occludes canal ,conductive deafness

Examination-
- primary lesion is often a small pustule that may enlarge to become a furuncle
- edema, erythema, tenderness and
- fluctuance if abscess forms
- periauricular lymph nodes enlarged & tender
treatment-
- early stages(without abscess)-
- systemic antibiotics,
- analgesics,
- local heat,
- ear pack of 10% ichthammol glycerine (reduces edema)
- late stage(with abscess)- incision &drainage and same as above
Extension of the infection to the pinna and periauricular soft tissues may warrant parenteral antibiotic therapy.
{note:
since as you know that hair follicle present only in outer third of ear canal(cartilagenous part) furuncle occurs in outer part only
recurrent furunculosis - suspect diabetes as cause}
Diffuse otitis externa:
- can involve whole of canal ,tympanic membrane & pinna
- also known as ’swimmers ear’
cause
- The most common precipitant of otitis externa is excessive moisture. Excessive moisture removes cerumen and increases the pH of the external auditory canal, situations that provide a good setting for bacterial growth. and
- trauma (due to scratching ,vigorous cleaning unskilled instrumentation)
- both of the above two impair the canal's natural defenses,& allow bacterial entry into ear canal
- The most common causative organism is Pseudomonas species and Staphylococcus aureus. Other pathogens less commonly cultured include Proteus mirabilis, Streptococci species, coagulase negative Staphylococci, and various gram negative bacilli.
clinical features-
Acute otitis externa- Chief symptoms include Otolagia& Otorrhea.
can further be divided into
- preinflammatory:
The preinflammatory stage begins with itching, edema and a full sensation in the ear.
- acute inflammatory stages. It is again divided into mild, moderate, or severe.
- As the infection progresses increased itching and pain ensues with mild erythema and edema on physical exam, however the canal lumen remains patent with cloudy secretions.
- During the moderate phase, the itching and pain intensify, and although the lumen remains patent, significant edema and debris decrease its size. Secretions are noted to be exudative and more profuse.
- Finally, in the severe stage of the disease, the pain is usually intolerable and is often intensified by manipulation of the skin and soft tissue around the ear. The lumen of the EAC may be obliterated by edema, debris and purulent otorrhea.
- The auricle and periauricular soft tissues are often involved, and regional lymph nodes may become palpable.Fever may be present, but if it exceeds 38.3°C (101.0°F), more than simple local otitis externa should be considered. Lymphadenopathy just anterior to the tragus is common.
- In patients where the disease does not resolve after treatment, a subacute or chronic form may occur.
treatment:
- ear cleaning is very important
- analgesics like codeine or NSAIDs used
- topical antibiotics
- An aminoglycoside combined with a second antibiotic and a topical steroid such as neomycin, polymyxin B, and hydrocortisone used to be the most commonly prescribed topical antibiotic. However, caution must be used to watch for a hypersensitivity reaction to the neomycin and ototoxicity from the aminoglycoside. This preparation should not be used in cases of a perforated tympanic membrane, which is not always easy to determine in cases of otitis externa.
- Fluoroquinolones are not assoiciated with ototoxicity and ofloxacin is safe in cases of a perforated tympanic membrane.
- Ofloxacin otic is the drug of choice when a perforated tympanic membrane cannot be ruled out.
- Systemic Treatment.: Oral antibiotics are rarely needed but should be used when otitis externa is persistent, when associated otitis media may be present or when local or systemic spread has occurred. The latter should be suspected if the patient's temperature is higher than 38.3°C (101.0°F), if initial pain is severe or if regional lymphadenopathy of the preauricular or anterior or posterior cervical chains is present.
{note:Currently, the only ototopical drop approved by the FDA for use in an open middle ear is ofloxacin. }
Chronic Otitis externa: Is defined when the duration of the infection exceeds 4 weeks or when more than 4 episodes occur in 1 year.
clinical features-
- characterized by irritation & strong desire to itch.
- discharge is scanty &dry up to form crusts
- meatal skin thick & swollen
- rarely skin becomes hypertrophic leading to meatal stenosis (CHRONIC STENOTIC OTITIS EXTERNA)
{note: discharge in otitis externa is serous type & in otitis media is mucoid type (this is due to presence of mucous membrane in middle ear)
treatment:
- reduce swelling=10% ichthammol glycerine
- reduce itching=antibiotic & steroid cream
- chronic stenotic otitis externa=surgical procedures to enlarge and resurface the EAC, such as conchal meatoplasty, are indicated.
Malignant otitis externa:"Osteitis of the base of the skull,"
Necrotizing or malignant otitis externa is a life-threatening extension of external otitis into the mastoid or temporal bone.
Known as Malignant due to high risk of Complications.
Aetiology-
- Most commonly caused by Pseudomonas aeruginosa, (98%)
- occurs most often in elderly patients with diabetes mellitus. However, all immunocompromised patients, especially those with human immunodeficiency virus (HIV) infection, are at risk.
- begins as an acute otitis externa and frequently progresses to a skull base osteomyelitis with resultant cranial neuropathies.
Clinical features-
- The typical patient is an elderly diabetic with poor metabolic control and evidence of otitis externa not responding to the usual local therapy.
- The typical complaints are deep-seated aural pain, discharge, and fullness.
- A history of diabetes or an immunocompromised state (neoplasm, immunosuppressive therapy, HIV, etc.) should be elicited.
- Examination of the involved ear canal reveals inflammation and granulation tissue at the bony cartilaginous junction. Purulent secretions are common, and excessive inflammation may occlude the canal and obscure the TM
{note:One of the hallmarks of necrotizing external otitis is granulation tissue in the external auditory canal, especially at the bone-cartilage junction.}This otoscopic finding is of extreme importance.
- The infection may extend to the cartilaginous skeleton of the ear canal and through Santorini's fissures to reach the temporal bone, causing osteitis. One of the hallmarks of this extension is granulation tissue in the bone-cartilage junction of the external auditory canal.
- Cranial nerve involvement may appear as early as one week after the onset of symptoms, with the facial nerve most commonly involved, followed by X and XI.
Diagnosis
Special alertness is required when external otitis is refractory to treatment and patients complain of severe otalgia, especially at night. The diagnosis of necrotizing external otitis is based on the clinical presentation and confirmed by laboratory tests and imaging studies.
LABORATORY TESTS
Mandatory laboratory tests include an erythrocyte sedimentation rate (ESR), white and red blood cell counts, glucose and creatinine levels, and culture of ear secretions. The ESR is typically elevated in necrotizing external otitis; therefore, it is a useful indicator of treatment response. Before topical or systemic antibiotic therapy is started, ear secretions should be cultured, because susceptibility patterns may change after the initiation of treatment (i.e., bacteria might become resistant to an antibiotic during treatment).Pathologic examination of granulation tissue removed from the external auditory canal is essential to exclude malignant processes, which may present as nonresponding inflammatory disease.
IMAGING STUDIES
Imaging to prove the extension of infection to bony structures is generally necessary to establish the diagnosis of necrotizing external otitis.
Imaging modalities include
- computed tomographic (CT) scanning,
- technetium Tc 99m medronate methylene diphosphonate bone scanning, and
- gallium citrate Ga(gallium) 67 scintigraphy.
CT scanning is used to determine the location and extent of diseased tissue.
- The temporal bone is the first bone to be affected, with imminent involvement of the petrous apex and mastoid.
- Extratemporal bone extension has become rare since the introduction of powerful antibiotics.
- In evaluating the CT scan, it is important to remember that at least one third of bone mineral must be lost before radiologic changes become apparent; conversely, bone remineralization continues long after the infection is cured.
- Thus, as related to the infectious process, pathology is late to appear on the CT scan and late to disappear.
- These factors limit the usefulness of CT scanning as a follow-up tool.
Tc(technitium) 99m bone scanning:
- Both osteoclasts and osteoblasts absorb 99mTc.
- Hence, bone scanning can locate a pathologic process in bone but is not informative about the nature of the process (infectious or other).
- Because the 99mTc scan remains positive as long as bone repair continues, this imaging modality is not helpful in follow-up.
gallium citrate Ga(gallium) 67 scintigraphy. :
- Since 67Ga is absorbed by macrophages and cells of the reticuloendothelial system, scanning with this radioisotope is a sensitive measure of ongoing infectious process .
- If 67Ga scintigraphy is available, it should be used for initial diagnosis and as a follow-up tool.
- By using imaging modalities in combination, it is possible to prove that the temporal bone is afflicted (CT scanning and 99mTc bone scanning) with an infectious process (67Ga scintigraphy).
Treatment:
- The excellent antipseudomonal activity of fluroquolones has generally made them the treatment of choice for necrotizing otitis externa,
- although a combination of a beta-lactam antibiotic and aminoglycoside is also effective.
- In severe cases, a prolonged course of parenteral antibiotics may be needed, but the excellent gastrointestinal absorption of the fluoroquinolones allows milder infections to be treated with a two-week course of oral therapy.
- Treatment should also include surgical debridement of any granulation or osteitic bone
otomycosis:
cause-
- aspegillus niger ,
- aspergillus fumigatus ,or
- candida albicans.
The most common pathogen is Aspergillus (80 to 90 percent of cases), followed by Candida.
Classically, fungal infection is the result of prolonged treatment of bacterial otitis externa that alters the flora of the ear canal. Mixed bacterial and fungal infections are thus common
Clinical features :
- the most common symptoms of otomycosis are pruritus deep within ear& an irresistible urge to scratch.
- The itching generally progresses to dull pain with or without drainage.
- The accumulation of fungal debris in the inflamed, narrowed canal often leads to a complaint of hearing loss.
- Tinnitus is also a common presenting complaint.
- however, with severe infections pain will also occur
examination with otoscope:Physical examination generally demonstrates canal erythema, mild edema and the presence of white, gray, or black fungal debris within the canal.
fungal mass is seen as "wet piece of filter paper"
- A.niger-black headed filamentous growth.

- A.fumigatus-pale blue or green
- Candida-white or creamy deposit.

treatment:
- Cleansing of the ear canal by suctioning is a principal treatment.
- Acidifying drops, given three or four times daily for five to seven days, are usually adequate to complete treatment.
- Because the infection can persist asymptomatically, the patient should be reevaluated at the end of the course of treatment. At this time any further cleansing can be performed as needed. If the infection is not resolving, over-the-counter clotrimazole 1 percent solution (Lotrimin), which also has some antibacterial activity, can be used
- Nystatin is effective against candida
Herpes Zoster Oticus (Ramsay Hunt syndrome) -some information taken from drtbalu wonderful educational site on ENT.
Ramsay Hunt syndrome is a disease affecting the external auditory canal associated with the following symptom complexes:
1. Lower motor neuron type of facial nerve palsy
2. Herpetic blisters of the skin of the external auditory canal
3. Otalgia
Pathophysiology:
The primary pathophysiology is located in the geniculate ganglion of the facial nerve. Geniculate ganglion is found to be affected by Human Herpes virus type 3 i.e. (Varicella zoster virus). Varicella zoster virus have been identified from tears of these patients by polymerase chain reaction. Infact Varicella zoster virus have also been identified from tears of patients with Bell's palsy.
Clinical features:
The classic Ramsay Hunt syndrome is associated with
1. Patient has deep seated pain in the affected ear. The pain is intermittent in nature, radiating towards the pinna of the ear. There is associated diffuse dull aching background pain.
2. Vertigo and ipsilateral hearing loss,
3. Tinnitus, and
4. Facial palsy (LMN type).

5. Rash or blisters can also be seen along the distribution of nervus intermedius. These herpetic blisters in the external auditory canal may become secondarily infected causing cellulitis.

Treatment:
1. Steps towards alleviating pain: Carbamazepine can be prescribed in doses of 400 mg / day in divided doses. Temporary relief of Otalgia in geniculate neuralgia may be achieved by applying a local anesthetic or cocaine to the trigger point, if in the external auditory canal.
2. Corticosteroids and oral acyclovir can be administered. Steroids in the form of prednisolone can be administered orally in doses of 10mg twice a day. Steroids should not be stopped abruptly. The dosage needs to be tapered. Acyclovir can be administered in doses of 800 mg orally 5 times a day.
3. Management of vertigo: can be managed using meclizine in doses of 25 mg orally 4 times a day.
4. Care must be taken to prevent exposure keratitis because of the inability to close the eye lids. The patients must wear protective goggles.
Acute (bullous) and chronic (granular) myringitis :
Acute myringitis is usually caused by a mycoplasma or viral infection and is observed in adults and children.
It is characterized by hemorrhagic bullae involving the tympanic membrane and a flulike syndrome.
It is self-limiting and requires pain and fever management.
Chronic myringitis is defined as de-epithelization of the tympanic membrane, granulation tissue formation, and discharge.
Treatment includes topical application of eardrops, a caustic solution in unresponsive cases, and mechanical removal of polypoidal granulations.
Eczematous otitis externa:
aetiology-hypersensitivity to infective organisms or topical ear drops such as neomycin
clinical features -irritation, vesicle formation, oozing & crusting.
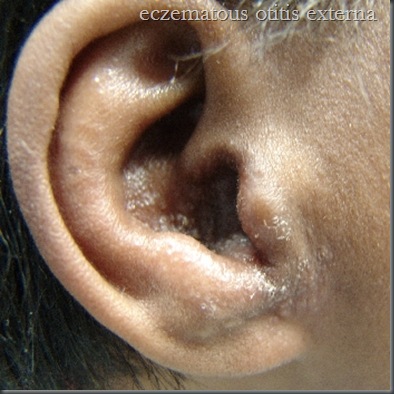
The dermatitis is generally confined to the site of contact with the allergen
treatment-withdrawal of agent causing it & application of steroid cream.
Seborrhoeic otitis externa:
Associated with Seborrhoeic dermatitis (dandruff) of scalp
Malassezia furfur, a lipophilic yeast, is thought to play at least some role in the development of this condition.
clinical features- itching
- greasy yellow scales in canal ,over lobule & postauricular sulcus.
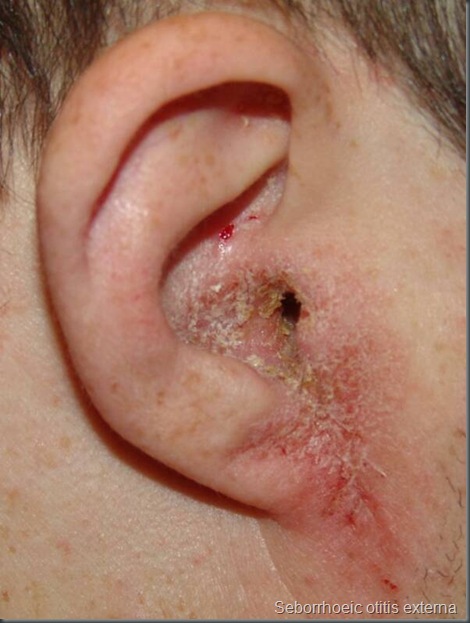
treatment-
- ear cleaning
- cream containing salicyclic acid & sulphur
- treat dandruff
Neurodermatitis:
cause-urge to scratch due to psychological reasons
clinical -
- only complaint is itching
- this may lead to secondary bacterial infection
treatment-
- sympathetic psychotherapy & treat secondary infection
- ear pack or bandage to prevent scratching
95 comments:
Hi,
I have been having episodes of severe pain in my left ear. This began October 2008. I have been to the doctor several times and was told that he could not see any signs as to why I would have this pain. I have been keeping a diary as advised by the doctor to write down when each episode occurrs. When it does, i take panadol. The pain has worseend over these months with an attack of pain 7 days ago which I found to be the most severe. It was at the point where walking and turning my head, the pain was unbearable. I have about two episodes a week now where it used to be about four times per month. Would you have any idea what the problem could be. Please help. My last attack was on Friday, and then today this afernoon. The pain starts to come on and then gradually worses, sometimes not to severe and other times where so severe that I have to pull over in my car and wait for the pain to ease off. At these times, it often hurts to walk and just have to see it through. Thankyou for reading my Comment,
Sincerely, Martha
I am still a medical student Madam,so probably you could seek help at http://www.netdoctor.co.uk
thank you! this is very informative. i'm a medical student from malaysia
excellent!am a med studnt frm india
thank you.im a medical student in hyderabad.india.
Hi,
I am writing this comment from Toronto, Canada.
I've been diagnosed with several chronic illnesses since 1994. In March 2012 I developed a strong kind of noise (like a river running over the left ear. I've seen 6 different ear doctors at different hospitals and all prescribed antibiotic, drops, nasal sprays, etc... The diagnose was the same, an inner ear some sort of infection.
Nothing taken helped even a bit, the river kind of noise associated with periods of change of intensity persisted, same times getting worst.
The director of the hearing clinic of the Toronto General Hospital suspected an inflammation of the meninges membrane close to the left ear. The swelling induced by the inflammation was eventually the cause. He suggested to start a treatment with 50mgs of Prednisone. As I have a certain intolerance to dosages in excess of 30mgs, the final decision was to start with 30mgs decreasing 2,5mgs weekly.
At the end of the 1st week all symptoms disappeared and my life became wonderful.
I want to share this story knowing that 98% of all MD's around this world don't know how to address this condition. They always wrongly diagnose infections, otitis, etc...
I recommend people suffering from auto-immune diseases(specially lupus) to discuss this with their doctors.
Good luck to everybody.
COMPLETE CURE TO TINNITUS: I had tinnitus in both ears for fifteen years with a high pitched two tone sound, the noises are constant and have learned to ignore the ringing. Later, another sound was added, a deep tone that has a sporadic rhythm, that mimics human speech. It varies from soft and muted, to painfully clear, and loud. Have try sound machines, ear plugs, my hearing aid, and medication all to no avail rather I have a difficult time sleeping. Lately I was directed to a Doctor called William on internet who provided solution to the problem. Do not be discourage, dr williams product is a permanent cure to Tinnitus. Contact him with this email (drwilliams098675@gmail.com)
Ear wicks are made by several different companies, namely Otocell and Americell brands. After inserting the wick, then apply the ear drops to it. headphones and tinnitus
Hi Nice Post,For More Updates
Best ENT Hospital in Hyderabad
• This is real take it serious, i am JOHNSON JUDITH i am from Ireland. Who will believe that a herbal medicine can cure HIV/AIDS, I never believe that this will work, i have spend a lot money getting drugs from the hospital to keep me and my son healthy, it got to a point that i was waiting for death to come because i was broke, one day i heard about this great man called Dr ODUWA who is well known for Herpes, HIV, and Cancer cure, i decided to email him I didn't believe him that much, I just wanted to give him a try, he replied my mail and Needed some Information about me, then I sent them to him, he prepared a herbal medicine (CURE) and, he gave my details to the Courier Office. they told me that 4-8 days I will receive the package and after receiving it, i took the medicine as prescribed by him at the end of the two weeks, he told me to go to the hospital for a checkup, and i went, surprisingly after the test the doctor confirm me HIV/AIDS negative, and my son and i thought it was a joke, i went to other hospital and was also negative, thank you for saving our life's, I promise I will always testify of your good works. If you are HIV/AIDS patient, contact him and I am sure you will get cured, contact him via: dr.oduwaspellhome@gmail.com or whatsapp him at +2348070685053.
THESE ARE THE THINGS Dr ODUWA CURE
. COLD SORE
. HIV/AIDS
. CANCER
. HPV
. LASSA FEVER
. GONORRHEA
Hi Nice Post,For More Updates
Best ENT clinic in Manikonda
I am Shelley from Los Angeles,California, I want to testify on how i got cured from tinnitus, I have suffered from ringing ears since the year 2011 with so mush pain,that i have to spend so mush money getting pain relief in the hospital, and I have visited several doctor ,but all to no avail, my world was gradually coming to an end because of the buzzing sound in my right ears, until i saw a post in a health forum about a herbal Dr Williams who use herbal portion in curing people from different kind of diseases including tinnitus, at first i doubted if it we be able to cure me, but i decided to give it a try, when i contacted this herbal doctor via his email, he prepared a herbal portion and sent it to me via courier service, when i received this herbal medicine, he gave me step by step instructions on how to apply it, when i applied it as instructed, i was completely free from tinnitus just for 1 months of usage,i we recommend this to all my friend family in the world today who still suffering from tinnitus you can contact him through his email on drwilliams098675@gmail.com for help.
hello to everyone out there, i am very happy to testify and inform the general public that I am finally cured from tinnitus infection totally with the use of a powerful herbal medicine, from a great herbal doctor i contacted through his email drrobinsonspellhome@gmail.com the powerful herbal medicine cured me totally and i was tested negative after usage, I am using this means to inform other's people who have the same infection virus, that there is a cure for tinnitus It is absolutely true. I was cured by Dr Robinson i advice you if you have tinnitus or any kind of deadly disease you can Contact him for help and get totally cured by his powerful herbs at drrobinsonspellhome@gmail.com
I am sophie from Canada, I once suffered from a terrible and Chronic tinnitus ,in 2016, the doctor told me it has no permanent cure i was given medications to slow down its progress, i constantly felt my health was deteriorating as i constantly go out of breath,and this noise was really terrible especially when am sleeping, i have this constant ringing in my ears for about 8 months, this was really a terrible noise ,on thin one day that i was going through the internet,and i came across a post of Mrs Kate on how she was been cured from tinnitus through dr Williams herbal product, I contacted this herbal doctor via his email and explain everything to him and make purchase of his product,few days later he sent me the herbal medicine through courier service, when i received the herbal medicine i used it for 3 weeks as prescribed and i was totally cured of tinnitus within those week of usage,on thin now i have not hear anything ringing in my ears.if you need his help you can Contact this herbal doctor via his email drwilliams098675@gmail.com for help
I'm here to testify about the great work Dr ogden did for me. I have been suffering from (HERPES) disease for the past 5 years and had constant pain, especially in my knees. During the first year,I had faith in God that i would be healed someday.This disease started circulating all over my body and i have been taking treatment from my doctor, few weeks ago i came across a testimony of one lady on the internet testifying about a Man called Dr ogden on how he cured her from Herpes Simplex Virus. And she also gave the email address of this man and advise anybody to contact him for help for any kind of sickness that he would be of help,so I emailed him on drogdentestimony@gmail.com telling him about my (HERPES Virus) he told me not to worry that i was going to be cured!! Well i never believed it,, well after all the procedures and remedy given to me by this man few weeks later i started experiencing changes all over me as Dr ogden assured me that i will be cured,after some time i went to my doctor to confirmed if i have be finally healed behold it was TRUE, So friends my advise is if you have such sickness or any other at all you can contact Dr ogden via email drogdentestimony@gmail.com You can also call or whatsApp his telephone number on +2348117963221.Thanks once again Dr ogden
I can’t believe this is really true I never believe there is cure to this hsv 2 because all the hospital have told me there is no cure to it, few months ago I saw this man email DR.AZIEGBE on internet from a testimony share by someone who he help with his herbal cure I contact his email and ask for his help also, that is how he inform me about the cure process and this man sent me a herbal medicine which I took according to the way he instructed for 2 week I can’t believe when I go for test my result come out negative i am so happy to share this to the world there is real cure to herpes you can also contact DR.AZIEGBE through his email now DRAZIEGBE1SPELLHOME@GMAIL. COM and also WhatsApp him +2349035465208. or my assistant whatsApp me +1 (601) 452-8622 or email: JAMESAVA0001@GMAIL. COM...
He also have herbs medicine to cured the following diseases;
Diabetes, Lupus, HPV, Gout, Hepatitis A,B, Infertility, HIV/AIDS, CANCER
Thanks for dharing such an impressive Information..keep sharing
Excellent information ,thank you for providing Ent Hospital In Kukatpally
Hello my dear viewers,I want the world to celebrate with me on this numerous testimony, i never believe i could ever get rid of this horrible disease until one fateful day,my story and appreciation goes to Dr.Akuza the powerful great doctor that help me to cure my HIV/AIDS disease from my life,he is truly a truthful man with high herbs power's he uses on saving people's life, just a few days back i came in contact with Dr.Akuza emails which many individuals have testify so much about of his kind work, so i decided and contacted him quickly because the disease was almost at the last minute of taking my life, i have tried all remedies from several physicians from hospitals but none could help me apart from Dr.Akuza who finally cure my HIV/AIDS disease, i was amazed and overwhelmed when the doctor confirmed me negative in the same hospital i have been before,i wish to anyone that is sick today and want healing to please contact this doctor on his Email akuzasolutionhome@gmail.com so if you have any problem HIV, HERPES, CANCER, ALS,HEPATITIS B, DIABETIC, call or whatsapp him on +2349035850834
great information
best hospital in kukatpally
I was despondent because i had a very small penis, about 2.5 inches soft and 4 inches hard not nice enough to satisfy a woman, i have been in so many relationship, but cut off because of my situation, i have used so many product which doctors prescribe for me, but none could offer me the help i searched for. i saw some few comments on the INTERNET about this specialist called Dr movo and decided to contact him on his email: {drmovo.supernaturalherbalmedic@gmail.com} so I decided to give his herbal product a try. i emailed him and he got back to me, he gave me some comforting words with his herbal pills for Penis Enlargement, Within 3 week of it, i began to feel the enlargement of my penis, " and now it just 4 weeks of using his products my penis is about 9 inches longer, and i had to settle out with my Ex girlfriend JOY, i was surprised when she said that she is satisfied with my sex and i have got a large penis. Am so happy, thanks to Dr movo I also learn that Dr movo also help with Breast Enlargement Hips and Bums Enlargement etc.. If you are in any situation with a little Penis, weak ejaculation, small breast_hips_bums do get to Dr movo now for help on his email:{drmovo.supernaturalherbalmedic@gmail.com} or whatsapp +2347061865209.
My name is Gwen Stacy Wailker , am here to appreciate Dr isiramen for using his herbal medicine to cure my Herpes virus. Is about 3 years and 6 months now I have been living with this virus and it has been a serious problem to me, I was so confused cause i have been taking several drugs to be cured but all of my effort was in vain,one morning I was browsing through the internet then I saw several testimonies about Dr. isiramen curing people from Herpes virus and immediately i contacted Dr. isiramen on his email: oyimeanelisiramen@gmail.com i told him about my troubles and he told me that i must be cured, he gave me some instructions and which i rightly followed. so he prepared a herbal medicine and sent it to me which i used for 2 weeks and i was cured everything was like a dream to me and my Herpes virus was totally gone, dr .isiramen, God bless you and give you more power and ability for more cure.I don't know if there is any one out there suffering for herpes virus or any of these diseases..DIABETES, CANCER, HIV/AIDS, HERPES HEPATITiS A AND B DISEASES etc. why don't you contact dr.Akhigbe today and be free from your diseases because he is very good and honest Doctor and he is also called the godfather of herbalism contact him via email; oyimeanelisiramen@gmail.com or whatsApp him on +234117963221
Ear wax, also known as cerumen, is produced in the ear canals by glands. Ear wax acts as part of the ears natural defence system preventing infection due to antibacterial agents. Its moist sticky properties also catch dust, debris and foreign objects which enter the ear.
How can I explain this to the world that there is a man who can cure HERPES, I was diagnosed for the past 5 mouth I have being into HERPES since 5 mouth, so I decide to look for help in the internet then I found a post write about this great man called DR. Agbonhale , people say good thing about him that this man have cured, a lot of people in the internet, him has power's to cure HSV1 AND HSV2 I don’t believe that there is a cure for Herpes Simplex Virus because though there is no cure for herpes that what I have in mind HERPES had no cure well , my HERPES is negative through the using of herbal cured of DR Agbonhale , I contacted this man for help because of what i see in the internet. if you need his cured just email him now on dragbonhaleherbalhome@gmail.com , thank you DR. i will never stop shearing you testimony DR. Agbonhale . him Can as well CURE THE FOLLOWING DISEASE:-1, HIV/AIDS, 2, Diseases of the hear 3, Malignant tumors 4. Cardiovascular diseases 5. Diabetes mellifluous 6.Influenza and pneumonia 7.Alzheimer's disease 8. hsv1 - hsv2. If you need LOVE SPELL. E.T.C contact him dragbonhaleherbalhome@gmail.com or you whatsapp him on +2349073130326.}
I have been suffering from (HERPES SIMPLEX VIRUS) disease for the past one years and had constant pain, especially in my knees. During the first year,I had faith in God that i would be healed someday.This disease started circulating all over my body and i have been taking treatment from my doctor, few weeks ago i came on search on the internet if i could get any information concerning the prevention of this disease, on my search i saw a testimony of someone who has been healed from (HERPES SIMPLEX VIRUS) by this Man Dr Agbonhale and she also gave the email address: dragbonhaleherbalhome@gmail.com of this man and advise we should contact him for any sickness that he would be of help, so i wrote to Dr. Agbonhale telling him about my (HERPES Virus) he told me not to worry that i was going to be cured!! hmm i never believed it,, well after all the procedures and remedy given to me by this man few weeks later i started experiencing changes all over me as the Dr Agbonhale assured me that i have cured,after some time i went to my doctor to confirmed if i have be finally healed behold it was TRUE, So friends my advise is if you have such sickness or any other at all you can email:: dragbonhaleherbalhome@gmail.com or whatsApp his number on +2349073130326..
Its a pleasure for me to write this testimony about how i got my Genital Herpes cured a month ago. i have been reading so many comments of some people who were cured from various diseases by Dr .Agbonhale, but i never believed them. I was hurt and depressed so I was too curious and wanted to try Dr. Agbonhale , then i contacted him through his email when i contact him, he assured me 100% that he will heal me, i pleaded with him to help me out. My treatment was a great success, he healed me just as he promised. he sent me his medication and ask me to go for check up after one weeks of taking the medication. i agreed with him i took this medication and went for check up a , to my greatest surprise my result was negative after the treatment, i am really happy that i am cured and healthy again. I have waited for 3weeks to be very sure i was completely healed before writing this testimony. I did another blood test one week ago and it was still Herpes negative. so i guess its time i recommend anyone going through Herpes HSV-1 or HSV-2, HIV, HPV, Hepatitis B, Diabetes, Cancer reach him through Email dragbonhaleherbalhome@gmail.com OR add on whatsapp +2349073130326.
What else can I say about him, today am very grateful to him as I am finally cured of herpes disease that I have been eating me up for over a year and 6 months.After searching for different means to get my self cure but nothing seems to work out,Behold today i can boldly stand and testify to the world at large that with the help of an herbal medicine,I have found myself back to my feet and healthy again in just after few days that i got in contact with a GOD sent man,through help on a blog which talk about herpes cure,how she was cured through the herbal medicine too which was sent to her from doctor Dr Adeola.So i decided to give this great man a try by contacting him via his email and mobile no,explained to him what my problems his and he told me all would be fine and well by the time he his done with is own work that i just have to believe in him which i did ,low and behold,today i am very happy as it was just all like a magic that is why i have come here to testify to the world at large and also to share my experience because I know there are many people out there who are also in searching for cure to one disease or the other,you can as well get Dr Adeola the great now for herbal medicine help through his contact address on dradeolaherbalhome@gmail.com also on mobile wha'sapp no +2349027752454 as i fully believe he is able and capable also getting rid of disease like
HIV/AIDS
HPV
CANCER
ALS .
i was diagnosed with Herpes for 2years ago i lived in pain with the knowledge that i wasn't going to ever be well again i contacted so many herbal doctors on this issue and wasted a large sum of money but my condition never got better i was determined to get my life back so one day i saw mis sanders post on how Dr Agbonhale saved him from the VIRUS with his herbal medicine i contacted Dr Agbonhale on his email address dragbonhaleherbalhome@gmail.com we spoke on the issue i told him all that i went through and he told me not to worry that everything will be fine again so he prepared the medicine and send it to me through courier service and told me how to use it,after 14days of usage I went to see the doctor for test ,then the result was negative,am the happiest woman on earth now. this testimony is real.thanks to Dr Agbonhale God bless you. you can also reach him on his whatsApp number +2349073130326.
Small amounts of wax in the ear canals are normal and keep the ear healthy. Large build ups of wax can cause the ears to become blocked.
Common symptoms of excessive wax include; pain, feeling of fullness, itching, ringing and partial/complete hearing loss.
Am really happy that i am cured of (HERPES SIMPLEX VIRUS) with the herbal medicine of Dr LUCKY , i have been suffering from this disease for the past 3 years without solution until i came across his email of this doctor who have cure so many people with his herbal medicine, i also choose to give him a chance to help me and my husband, he told me what to do and i kindly did it, and he gave us his herbal medicine and direct me on how to use it, i also follows his instruction for use and he ask us to go for a check up after 3 weeks and which i did, to my greatest surprise our result came out as negative, we are really happy that there is someone like this DR LUCKY who is ready to help anytime any day. to all the readers and viewers that is doubting this testimony stop doubting it and contact this Dr and see if he will not actually help you. i am not a stupid woman that i will come out to the public and start saying what someone have not done for me .contact him now if you are also in need of help via email;( drluckyherbalcure@gmail.com ) call or whatsapp +2348154637647 may bless you sir for all your good works. contact Dr LUCKY today for your following diseases below HIV/AIDS DIABETES HPV PENIS ENLARGEMENT BRAIN TOMOUR
I still don’t know the right words to express my gratitude to this great man Dr Isibor. After been diagnosed of HERPES SIMPLEX VIRUS in 2months ago, i was given so many health prescription and advice with no improvement, I totally lost hope, until i found testimonies of Great Dr Isibor online research and on Facebook, Like anybody would be, I was very skeptical about contacting him, but i later did and he opened up to me and told me what was involved and he started the remedies for my health. Thank God, i was cured from herpes by the herbal medication I received from him. I never thought that herpes can be cured, from the bottom of my heart I'm truly grateful,i pray you have long life so you can help many more people on earth with your herbal medical support, You can Email him via email drisiborspellhome@gmail.com or for easy and fast communication you can also call or add him on whats-app with this mobile number +2348107855231, one thing i love most about DR Isibor is honestly, and he is very polite with his patience, everything he told me what he did, and his herbal medicine are very affordable.
Dr ohunyom herbal medicine is a good remedy for herpes simplex virus cure. My name is donald Joe ,I just want to share this article about Dr ohunyom who helped me, i want to inform the public how i was cured from (HERPES SIMPLEX VIRUS) by DR ohunyom, i visited different hospital but they gave me list of drugs like Familiar , Zovirax, and Valtrex which is very expensive to treat the symptoms and never cured me. I was browsing through the Internet searching for remedy on HERPES and i saw comment of people talking about how DR ohunyom cured them, when i contacted him he gave me hope and send a Herbal medicine to me that i took and it seriously worked for me, am a free person now without any problem, my HERPES result came out negative, I pray to God to never let me and my family forget you in our life,i am now cured permanently.you can also get your self cured, if you really need this dr's help,you can reach him now email:drohunyom@gmail. com Or whats app +2349060579973
This is real,
He also has herbal cure for the Following DISEASES, eczema,urethra wart,chronic problems.Herpes, Cancer, Als,Hepatitis, Diabetes, HPV,Infections,ulcer ETC
My boyfriend and I met three years ago on herpes dating site so we discovered we are +ve from the beginning of our relationship, that we both had genital herpes. My first outbreak was the ABSOLUTE worst experience, I was so sick. We suffered for one year plus, had constant outbreaks and then finally we decided to both respectively take Dr Utu African Traditional Herbs as advised by friends. His herb is Not much bitter or sour taste.
Dosage two times daily every day for four weeks, and honest to goodness it was a miraculous herbs. We were on it for not more than two weeks when we noticed total change. 'couldn't wait for four weeks. It was third week and five days we used the herbs. Then we went for test and was already hsv2 negative, the both of us. Neither of us have had any lesion, outbreak or symptoms till date.
For traditional and permanent hsv cure, Contact him on drutuherbalcure@gmail.com or direct WhatsApp or phone +2347032718477
God bless Dr. Momoh for his marvelous work in my life, I was diagnosed of HIV since 2010 and I was
taking my medications, I wasn't satisfied i needed
to get the HIV.out of my system, I searched about
some possible cure for HIV i saw a comment about, how he cured HIV with his herbal
medicine, I contacted him and he guided me.I
asked for solutions, he started the remedy for my
health, he sent me the medicine through UPS SPEED
POST.I took the medicine as prescribed by him
and 14 days later i was cured from HIV, thank you so much and you are the one that God sent to change my miserable life, you the almighty god be with you all the days of your life, so my brothers and sisters we cancontact him on this email address.dr.momoh9@gmail.com or whatsapp him on +2347083724098 Dr momoh ONCE AGAIN
THANK YOU SIR.
Dr momoh he also told me that he can cure the flowing virus,
1 cancer cure
2 diabetes cure
3 ringing ear
4 herpes cure
5 warts cure
6 HPV cure
7 get your ex back
8 pregnancy herbal medicine
9 prostate enlargement
10 Hepatitis B
So is possible that HIV Disease can be cured because I have been scammed so many times not until I came across this great man Dr Akhigbe who helped me at first I never believe all this comment and post about him and I was very sick because I have been infected with HIV/AIDS for the past two year,just last 2 months I keep reading the testimony about this man named Dr Akhigbe they said that the man is so powerful he have cured different type of diseases, I keep monitoring his post of some people about this man and I found out that he was real so I decided to give him a trial I contacted him for help and he said he was going to help me get my cure that all I needed to do was to send him money to prepare the medication after which it will be sent to me via DHL courier delivery services which I did to my greatest surprise the medication was sent to me he gave me instructions to follow on how to drink it that after three weeks I should go for check up,after taking the medicine and follow his instruction after three weeks I went back to the hospital for another test, at first I was shocked when the doctor told me that I was negative I ask the doctor to check again and the result was still the same negative that was how I free from HIV VIRUS at of the shock I decided to come and share my own testimony with you for those who think there is no cure for HIV VIRUS the cure as finally come' out stop doubting and contact Dr Akhigbe via email drrealakhigbe@gmail.com he will help you out you can also whatsApp him via +2348142454860 he is also perfect in curing DIABETICS,HERPES,HIV/AIDS, ;ALS, CANCER ,HEPATITIS A AND B,ASTHMA, HEART DISEASE, CHRONIC DISEASE.,KIDNEY DISEASE, LUPUS,EXTERNAL INFECTION, EPILEPSY,STROKE, ECZEMA, EATING DISORDER etc believe me that deadly disease is not longer a deadly sentence because dr akhigbe has the cure.the godfather of herbal root.
email: drrealakhigbe@gmail.com whatsapp number.
+2348142454860
website: https://drrealakhigbe.weebly.com
Hello everyone! my name is Noah, I'm writing this article to appreciate the good work of DR AKHIGBE that helped me recently to bring back my wife that left me for another man for the past 6 months. After seeing a comment of a woman on the internet testifying of how she was helped by DR AKHIGBE I also decided to contact him for help because all i wanted was for me to get my wife, happiness and to make sure that my child grows up with his mother 'I love my wife' Am happy today that he helped me and i can proudly say that my wife is now with me again and she is now in love with me like never before. Are you in need of any help in your relationship like getting back your man, wife, boyfriend, girlfriend or loves and family relationship. Viewers reading my post that needs the help of DR AKHIGBE should contact him via E-mail: drrealakhigbe@gmail.com You can also call or contact him via whatsapp +2348142454860 He also cure deadly diseases and virus with his natural herbal medicine herbs. like
HIV/AIDS
HERPES
EPILEPSY
STROKE
EXTERNAL INFECTION
CANCER
DIABETES
CHRONIC DISEASE
HEPATITIS A&B AND OTHERS. his email again: drrealakhigbe@gmail.com
number : +2348142454860
Hello Everyone, I was suffering of Shingles since 2016 and I was taking my medications, I wasn't satisfied all i needed is to be permanently free from this disease, I searched about some possible cure for Shingles i saw a comment about Dr. OSEIBOH, how he cured Shingles with his natural herbal medicine, I contacted him at his email; droseiboh12@gmail.com and i got his response. I asked for solutions, all he said to me was that i should not worry that he will send me the remedy cure that i will apply to get rid of it permanently. He sent me the medicine. I took the medicine as prescribed by him, a week and some days later i was cured from Shingles all rashes were dried off, via email droseiboh12@gmail.com add him on whatsapp line or call +2347017565415. Dr OSEIBOH ONCE AGAIN THANK YOU FOR YOUR INSTANT HELP!!!
HE CAN ALSO CURE SICKNESS LIKE. HIV/AIDS,DIABETES,PREGNANCY,CANCER,HPV,ALS,HEPATITIS,LOVE SPELL.
I am LUCAS from Chicago i was diagnosed with Herpes Virus for over 12 years which made loose my job and my relationship with my fiance after he discovered that i was having Herpes Virus, he departed from me i tried all my best to make him stays with me, but neglected me until a friend of mine on Facebook from Singapore told me Great healer, who will restore my life back with his powerful healing spell, he sent me the email address to contact and i quickly contacted him, and he said my condition can solved, that he will treat the disease immediately only if i can accept trust him and accept his terms and condition, i Agreed because i was so much in need of help by all means, so i did all he want from me and surprisingly on Sunday last week He sent me a text, that i should hurry up to the hospital for a checkup, which i truly did, i confirm from my doctor that i no longer have herpes my eyes filled with tears and joy, crying heavily because truly the disease deprived me of many things from my life, This is a Miracle, Please do not en-devour to whatsapp Dr AJAGBO on (+2348055567537) Or email him via: drajagbookuta@gmail.com....
I am LUCAS from Chicago i was diagnosed with Herpes Virus for over 12 years which made loose my job and my relationship with my fiance after he discovered that i was having Herpes Virus, he departed from me i tried all my best to make him stays with me, but neglected me until a friend of mine on Facebook from Singapore told me Great healer, who will restore my life back with his powerful healing spell, he sent me the email address to contact and i quickly contacted him, and he said my condition can solved, that he will treat the disease immediately only if i can accept trust him and accept his terms and condition, i Agreed because i was so much in need of help by all means, so i did all he want from me and surprisingly on Sunday last week He sent me a text, that i should hurry up to the hospital for a checkup, which i truly did, i confirm from my doctor that i no longer have herpes my eyes filled with tears and joy, crying heavily because truly the disease deprived me of many things from my life, This is a Miracle, Please do not en-devour to whatsapp Dr AJAGBO on (+2348055567537) Or email him via: drajagbookuta@gmail.com....
Good day every one i want to inform the public on how i get cured of HIV/AIDS by a Doctor called OBUDU . i visited different hospital but they gave me list of expensive drugs to treat the symptoms and never cured me. A closed friend of mine introduce me to a Herbal Doctor who cured her. I was scared to contact him but i faund people testimony online testifying about his goodness. when i contacted him i asked him series of questions, i also ask him to show me his herbal certificate and license given to him by his Government he gave all the information i needed that gave me hope. He send a Herbal medicine to me that i took and it seriously worked for me. am now HIV negative. God bless you for being a sincere and great men. Am so excited, you can contact him if you have any problem whats-app +2347035974895.or contact him on email(OBUDU.MIRACLEHERBALHOME@GMAIL.COM)
And he can also cure the following diseases
1) HERPES
2) HPV
4) HEPATITIS
5) ALS
6) BLOOD CANCER
I know this could be disrespectful but i would still share my testimony with you all whom would also need same help, i got married to my wife 3 years ago until i came across DR AZIBA we could not have a child because my Penis was too small to perform and could not erect, this almost cost me my marriage, i wept in close door, no help coming , so i went online for a helpful research and i came across a review written about DR. AZIBA who prepares PENIS ENLARGEMENT PRODUCT and his contact details were also written on how he prepares root and vegetables natural product to help grow penis , so i applied and he send it to my address and instruct me on how to use, within the period of (7days) my penis is already growing from 3:5 to 6:5 and DR made it known to me that i can stop when am satisfied with the result, my dear friends this is worth celebrating and sharing with my fellow men same goes to women who needs this for there man, i will write down his contact details so you all can contact the DR AZIBA as well.
WhatsApp: +2348100368288
Email: Priestazibasolutioncenter@gmail.com
BREAST ENLARGEMENT
BREAST LIFT & REDUCTION
PENILE/PENIS ENLARGEMENT
GENERAL BODY SLIMMING
HIPS & THIGH REDUCTION
REGAIN VIRGINITY BACK
How can I explain this to the world that there is a man who can cure HERPES, I was diagnosed for the past 5 mouth I have being into HERPES since 5 mouth, so I decide to look for help in the internet then I found a post write about this great man called DR. Agbonhale , people say good thing about him that this man have cured, a lot of people in the internet, him has power's to cure HSV1 AND HSV2 I don’t believe that there is a cure for Herpes Simplex Virus because though there is no cure for herpes that what I have in mind HERPES had no cure well , my HERPES is negative through the using of herbal cured of DR Agbonhale , I contacted this man for help because of what i see in the internet. if you need his cured just email him now on dragbonhaleherbalhome@gmail.com , thank you DR. i will never stop shearing you testimony DR. Agbonhale . him Can as well CURE THE FOLLOWING DISEASE:-1, HIV/AIDS, 2, Diseases of the hear 3, Malignant tumors 4. Cardiovascular diseases 5. Diabetes mellifluous 6.Influenza and pneumonia 7.Alzheimer's disease 8. hsv1 - hsv2. If you need LOVE SPELL. E.T.C contact him dragbonhaleherbalhome@gmail.com or you whatsapp him on +2349073130326.
I almost gave up on ever getting cured of HIV VIURS because i have try many treatment none of them work out for me i have go to different hospital they always tell me same thing there is no cure for HIV when i came across a post about Dr OSAGIE, in the net from a lady called Angela i contacted him and he reassured me with him herbal medicine which i took according to the way he instructed, that how i was cured. I doubted at first because i have been to a whole lot of reputable doctors, tried a lot of medicines but none was able to cure me. so i decided to listen to him and he commenced treatment, and under two weeks i was totally fee from #HIV V`IURS i want to say a very big thank you to DR OSAGIE for what he has done in my life. feel free to leave him a message on email his email: (drosagiesolutiontemple@gmail.com OR
DROSAGIESOULTIONTEMPLE@YAHOO.COM ) and also WhatsApp him +2347030465649..
He can still be able to help you with this herbs medicine:
1...ALS CURE
DIABETES CURE
EPILESY CURE
HPV CURE
LUPUS CURE
HEPATITIS CURE
CANCER CURE
thank you my great dr .,,
Good day to all viewer online am so happy sharing this great testimony on how i was checking for solution in the internet then miraculously i came Across Dr.Oba the powerful herbalist that Cure Numerous individuals Herpes Simplex Virus,so I contacted him base on the testimonies I?m seeing about him on the internet, I was cured too by him, kindly contact him actoday through his email he can help you email ; drobaspellhome902@gmail.com OR WHATSAPP +2348088337602 and so he can cure types of diseases like,HEPATITIS B,DIABETICS,CANCER,HPV,LOW SPERM CAM HIV/STDS FIBROSIS LOST OF WEIGHT .. all thank to you Dr Oba for your kindly help in my life
OMG i am here to tell you all how i was cured from Hepatitis B by
dr Adigba with his herbal medicine i once had the problem of
Hepatitis B which affected my work for years i have been using
different medication but there was no solution,i search the net and
i found the contact of Dr Adigba who help me with his product on
curing Hepatitis B problem and other deadly diseases, he also
assured me that it is a permanent cure,so i work with him
as he ask
and i took the medication for just 1 weeks and i was back
to normal.
for two weeks now i have been doing fine.I give all thanks
to Dr
Adigba for helping me out of such problem now am the
happiest
person on earth for seeing myself doing better again.you
can also
contact him on email drAdigba@gmail. com whatsapp him
on +2348077875210
dr adigba cure the flowing virus
1 cancer cure
2 diabetes cureringing ear
3 ringing earwarts cure
4 herpes cure
5 warts cure
6 HPV cure
7 Jaundice
8 pregnancy herbal medicine
9 prostate enlargement
10 Hepatitis B and many more
Traditional Herbal doctor Zuku Cure HSV-2 Disease WhatsApp Number:+254742884656
I want to thank Dr ZUKU for helping me with his Herbal Medicine that cure my HSV-2 Disease completely.i have been living with HSV-2 Disease for the past 3yrs. i was so happy when i found Dr Zuku Blogs:https://drzukuspelltemple.blogspot.co.ke/ how Dr Zuku help people in the world.to cure HSV, with Herbal Medicine he Cured My HSV -2 Negative after using the Herbal Medicine Dr ZUKU sent to me. I give thanks to God and healed completely. you are the best Traditional Herbal doctor in the world Dr Zuku, WhatsApp Number:+254742884656 Contact Doctor Zuku Email drzukuspelltemple@gmail.com OR Contact Zuku Website: http://drzukuspelltemple.website2.me/
For those people whose relative are suffering from Tinnitus and maybe reading this, I find it hard that people are still ignorant of herbal medicine when it comes to treating Tinnitus. I have been through many phases over the last couple of years since my (audiological) exam/diagnosis, my tinnitus once buried me in a negative place where many of you are now - or have been. Believe me when I say, “I’ve been there.” I had sudden sensorineural hearing loss (SSHL), losing 70 percent of my hearing up to 4,000 kHz. I began noticing a low level of tinnitus around 51 years old and the diagnosis changed my life in many ways, I spend most of the time in denial and I keep thinking the tests were wrong. But deep down I knew they were correct. The level spiked dramatically, spiraling me down into a pit of depression. I could not sleep or eat; I stayed in bed with sweats and shaking spells; I lost strength and considerable weight. My wife held me in her arms, trying to comfort me, and still I thought I was going to die. Though sharing his story is very difficult. I was always very successful in being able to accomplish anything I set my mind on doing. Tinnitus is a bitch. I feel a need to express my thoughts and feelings about how it affected my day to day living and how its deteriorated since despite the help of some wonderful medics and medicine.
I remind myself how lucky to come across aparajita tan herbal medicine which is able to control Tinnitus without any side effect, I felt a moment of relief hoping that I am free from this ailment, and nothing compares to the healing power of nature. Now I believe almost every health problem can be addressed in one natural way or another. The only thing I wanted was for me to feel better. I’m proud to say am Tinnitus free. You can also contact him for advice and more info. aparajitatan@gmail.com
HELLO EVERYONE.. FEW MUNINETS TO REDY THIS INFOR ON HERPES CURE 2018..
2017 MY MOTHER WAS DIAGNOSED OF HERPES/ KNOWN AS GENITAL WARTS ,I SPENT A LOT OF MONEY ON HER MEDICATION TILL A POINT I EVEN LOST HOPE,BECAUSE MY MOTHER WAS GRADUALLY DYING AND LOST HER MEMORY TOO, I WAS SO DESPERATE TO GET MY MOTHER BACK TO NORMAL, ONE DAY MY UNCLE WHO LIVES IN LONDON UNITED KINGDOM TOLD ME ABOUT DR OLIHA ,WHO HELPED HIM GET RID OF HERPES /GENITAL WART WITH HERBAL MEDICINE AND HIS HERBAL SOAP ,I WAS SO SHOCKED WHEN HE TOLD ME ABOUT THIS ,ALTHOUGH I NEVER BELIEVE IN HERB BUT, I KEEP TO BELIEVE BECAUSE MY UNCLE CAN'T TELL ME LIES WHEN IT COMES TO HEALTH CONDITION I CONTACTED DR OLIHA VIA HIS EMAIL; OLIHA.MIRACLEMEDICINE@GMAIL.COM , YOU CAN TALK TO HIM VIA CALL OR WHATSAPP MESSENGER ON +2349038382931 , HE REPLIED AND ASK ME TO SEND MY HOME ADDRESS AND MY MOTHER'S DETAIL AND THEN I PURCHASED THE HERBAL MEDICINE,SENT ME THE HERBAL MEDICINE THROUGH COURIER SERVICE, WHEN I RECEIVED THIS HERBAL MEDICINE USED IT FOR 2 WEEKS, AND 4 DAYS OF USAGE THE WARTS FELL OFF, MY MOTHER I NOW TOTALLY CURED AND MY MOTHER IS LIVING FREE AND HAPPY AGAIN. YOU CAN TALK TO DR VIA HIS MOBILE NUMBER OR WHATS APP HIM ON +2349038382931.ALL THANKS TO DOCTOR DR OLIHA
HELLO EVERYONE.. FEW MUNINETS TO REDY THIS INFOR ON HERPES CURE 2018..
2017 MY MOTHER WAS DIAGNOSED OF HERPES/ KNOWN AS GENITAL WARTS ,I SPENT A LOT OF MONEY ON HER MEDICATION TILL A POINT I EVEN LOST HOPE,BECAUSE MY MOTHER WAS GRADUALLY DYING AND LOST HER MEMORY TOO, I WAS SO DESPERATE TO GET MY MOTHER BACK TO NORMAL, ONE DAY MY UNCLE WHO LIVES IN LONDON UNITED KINGDOM TOLD ME ABOUT DR OLIHA ,WHO HELPED HIM GET RID OF HERPES /GENITAL WART WITH HERBAL MEDICINE AND HIS HERBAL SOAP ,I WAS SO SHOCKED WHEN HE TOLD ME ABOUT THIS ,ALTHOUGH I NEVER BELIEVE IN HERB BUT, I KEEP TO BELIEVE BECAUSE MY UNCLE CAN'T TELL ME LIES WHEN IT COMES TO HEALTH CONDITION I CONTACTED DR OLIHA VIA HIS EMAIL; OLIHA.MIRACLEMEDICINE@GMAIL.COM , YOU CAN TALK TO HIM VIA CALL OR WHATSAPP MESSENGER ON +2349038382931 , HE REPLIED AND ASK ME TO SEND MY HOME ADDRESS AND MY MOTHER'S DETAIL AND THEN I PURCHASED THE HERBAL MEDICINE,SENT ME THE HERBAL MEDICINE THROUGH COURIER SERVICE, WHEN I RECEIVED THIS HERBAL MEDICINE USED IT FOR 2 WEEKS, AND 4 DAYS OF USAGE THE WARTS FELL OFF, MY MOTHER I NOW TOTALLY CURED AND MY MOTHER IS LIVING FREE AND HAPPY AGAIN. YOU CAN TALK TO DR VIA HIS MOBILE NUMBER OR WHATS APP HIM ON +2349038382931.ALL THANKS TO DOCTOR DR OLIHA
Am here to appreciate Dr Emmanuel for using his herbal medicine to cure my herpes virus. since 3 years now I have been living with this virus and it has been giving me challenges, I was so perplexed cause i have been taking several drugs to be cured but all of my effort was in vain,one morning i was browsing through the internet then i saw several testimonies about Dr. Emmanuel curing people from Herpes virus and immediately i contacted Dr. Emmanuel on his email: nativehealthclinic@gmail.com, i told him about my troubles and he told me that i must be cured, gave me some instructions and which i rightly followed. so he prepared a herbal medicine for me and sent it to me which i used for 2 weeks and everything was like a dream to me and my Herpes virus was totally gone, why don't you contact him today and be free from your diseases because he is very good and honest Doctor. contact him via email; nativehealthclinic@gmail.com or whatsApp/Call him on +2348140073965God bless him for me.he also cured HIV/AID,Sgenital ,wart,COPD,cancel and all kind of disease and virus
i want to inform the public how i was cured of HERPES Simplex Virus by a
Doctor called Dr.IRABOR. i visited different hospital but they gave me list
of drugs like Famvir, Zovirax, and Valtrex which is very expensive to treat
the symptoms and never cured me. I was browsing through the Internet
searching for remedy on HERPES and i saw comment of people talking about
how Doctor IRABOR cured them. I Was scared because i never believed in the
Internet but i was convince to give him a try because i was having no hope
of been cured of HERPES so i decided to contact him on his email, i
searched his email on net and i saw a lot of people testifying about his
goodness. when i contacted him he gave me hope and send a Herbal medicine
to me that i took and it seriously worked for me, am a free person now
without problem, my HERPES result came out negative. You can contact him on
his Email: driraborherbalhome@gmail.com call me+2348159922297 or whatsapp me +2348159922297 and get all your problem solved.
1)Sickness of any kind
2)Help to CURE Hepatitis B, HIV/AIDs CANCER and BIPOLAR
3)Divorce, Breakup problem and To Re-unit
4)Pregnancy problem
5)Financial problem and Job promotion
6)To get a good and rich life partner
7)To Lose your wath
8)to enlargement of pennis
9. CANCER
10. ALS (Lou Gehrig's disease)
11. Hepatitis B
12. chronic pancreatic
13. emphysema
14. COPD (chronic obstructive pulmonary disease)
Hello everyone, Now this is to everyone out there with different health challenges, as I know there are still a lot of people suffering from different health issues and are therefore looking for solution. I bring you Good news. There is a man called Dr RAZOR a herbal practitioner who helped cure me from Genital herpes, this i had suffered from for the past 2years and i have spent so much money trying to survive from it. I got my healing by taking the herbal medicine he sent to me to drink for about 18days after i got in touch with him through a friend of mine.3days after completion of the dosage, I went for a medical checkup and I was tested Genital Herpes NEGATIVE. I’m sharing this so that other people can know of this great healer called Dr RAZOR because I got to know him through a friend he cured from HIV. I was made to understand that he can cure several other deadly diseases and infections. Don’t die in ignorance and don’t let that illness take your life. Contact Dr RAZOR through his email ;drrazorherbalhome@gmail.com You can also call him on:+2349065420442 Thank you Dr RAZOR . Be kind enough to share as you received.
Chemicals used in industries gives me Leukemia Cancer and it's all started when I wanted to get off my job to get another job that when I got diagnose, at that very point I was so scared to die because it has infected my blood cells also I was prescribed drugs like Cyclophosphamide,Busulfan,Bosutinib,Cytarabine, Cytosar-U (Cytarabine),Dasatinib in all that was just to keep me waiting for my dying day. I got inspired by what I read from a lady called Tara Omar on blog spot on how Dr Itua cure her HIV/Aids then they were lettered below that says he can cure Cancer so I pick his contact on the testimony she wrote then I emailed Dr Itua hopefully he replied swiftly to my mail then I purchased his Herbal medicine also it was shipped to me here in Texas, I went to pick it at post office so he instructs me on how the treatment will take me three weeks to cure my Leukemia Disease, Joyfully I was cured by this Dr Itua Herbal Medicine.
I will advise you too to give a try to Dr Itua Herbal Medicine with the following diseases that he can help you cure forever___Diabetes, Herpes,HIV/Aids, Bladder Cancer, Breast Cancer, Parkinson's disease,Schizophrenia,Lung Cancer,Breast Cancer,Colo-Rectal Cancer,Blood Cancer,Prostate Cancer,siva.Fatal Familial Insomnia Factor V Leiden Mutation ,Epilepsy Dupuytren's disease,Desmoplastic small-round-cell tumor Diabetes ,Coeliac disease,Creutzfeldt–Jakob disease,Cerebral Amyloid Angiopathy, Ataxia,Arthritis,Amyotrophic Lateral Scoliosis,Fibromyalgia,Fluoroquinolone Toxicity
Syndrome Fibrodysplasia Ossificans ProgresSclerosis,Seizures,Alzheimer's disease,Adrenocortical carcinoma.Asthma,Allergic diseases.Copd,Glaucoma., Cataracts,Macular degeneration,Cardiovascular disease,Lung disease.Enlarged prostate,Osteoporosis.Alzheimer's disease,
Dementia.Vaginal Cancer, Kidney Cancer, Lung Cancer, Skin Cancer, Uterine Cancer, Prostate Cancer, Colo_Rectal Cancer, Leukemia Cancer, Hepatitis, Brain Tumors, Tach Disease,Love Spell, Infertility, Hpv. GoodLuck,XoXo****
Dr Itua Contact Information:::
Email (drituaherbalcenter@gmail.com)
WhatsApp-(+2348149277967)
have been using this herbal cure remedy for 3 months now. So far, it has cured my HEPATITIS B, eliminated my COLD SORE, improved energy and metabolism, in the morning I feel recharged and I no longer feel sleepy after a meal. As for the scent, it does smell like motor oil but I chase it down with 100% Cranberry Juice 1tsp. twice a day AFTER a meal. I also experienced vivid dreams for about 5 days now it's diminishing to during the first 2 or 3 hours of sleep . contact : EMAIL..DR. EKPEN doctorekpen222@gmail.coDm or call/whatsapp +2348102454875. you can get the cure from him and be free from all kinds of diseases
HELLO EVERYONE.. FEW MUNINETS TO REDY THIS INFOR ON HERPES CURE 2018..
2017 MY MOTHER WAS DIAGNOSED OF HERPES/ KNOWN AS GENITAL WARTS ,I SPENT A LOT OF MONEY ON HER MEDICATION TILL A POINT I EVEN LOST HOPE,BECAUSE MY MOTHER WAS GRADUALLY DYING AND LOST HER MEMORY TOO, I WAS SO DESPERATE TO GET MY MOTHER BACK TO NORMAL, ONE DAY MY UNCLE WHO LIVES IN LONDON UNITED KINGDOM TOLD ME ABOUT DR OLIHA ,WHO HELPED HIM GET RID OF HERPES /GENITAL WART WITH HERBAL MEDICINE AND HIS HERBAL SOAP ,I WAS SO SHOCKED WHEN HE TOLD ME ABOUT THIS ,ALTHOUGH I NEVER BELIEVE IN HERB BUT, I KEEP TO BELIEVE BECAUSE MY UNCLE CAN'T TELL ME LIES WHEN IT COMES TO HEALTH CONDITION I CONTACTED DR OLIHA VIA HIS EMAIL; OLIHA.MIRACLEMEDICINE@GMAIL.COM , YOU CAN TALK TO HIM VIA CALL OR WHATSAPP MESSENGER ON +2349038382931 , HE REPLIED AND ASK ME TO SEND MY HOME ADDRESS AND MY MOTHER'S DETAIL AND THEN I PURCHASED THE HERBAL MEDICINE,SENT ME THE HERBAL MEDICINE THROUGH COURIER SERVICE, WHEN I RECEIVED THIS HERBAL MEDICINE USED IT FOR 2 WEEKS, AND 4 DAYS OF USAGE THE WARTS FELL OFF, MY MOTHER I NOW TOTALLY CURED AND MY MOTHER IS LIVING FREE AND HAPPY AGAIN. YOU CAN TALK TO DR VIA HIS MOBILE NUMBER OR WHATS APP HIM ON +2349038382931.ALL THANKS TO DOCTOR DR OLIHA
HELLO EVERYONE.. FEW MUNINETS TO REDY THIS INFOR ON HERPES CURE 2018..
2017 MY MOTHER WAS DIAGNOSED OF HERPES/ KNOWN AS GENITAL WARTS ,I SPENT A LOT OF MONEY ON HER MEDICATION TILL A POINT I EVEN LOST HOPE,BECAUSE MY MOTHER WAS GRADUALLY DYING AND LOST HER MEMORY TOO, I WAS SO DESPERATE TO GET MY MOTHER BACK TO NORMAL, ONE DAY MY UNCLE WHO LIVES IN LONDON UNITED KINGDOM TOLD ME ABOUT DR OLIHA ,WHO HELPED HIM GET RID OF HERPES /GENITAL WART WITH HERBAL MEDICINE AND HIS HERBAL SOAP ,I WAS SO SHOCKED WHEN HE TOLD ME ABOUT THIS ,ALTHOUGH I NEVER BELIEVE IN HERB BUT, I KEEP TO BELIEVE BECAUSE MY UNCLE CAN'T TELL ME LIES WHEN IT COMES TO HEALTH CONDITION I CONTACTED DR OLIHA VIA HIS EMAIL; OLIHA.MIRACLEMEDICINE@GMAIL.COM , YOU CAN TALK TO HIM VIA CALL OR WHATSAPP MESSENGER ON +2349038382931 , HE REPLIED AND ASK ME TO SEND MY HOME ADDRESS AND MY MOTHER'S DETAIL AND THEN I PURCHASED THE HERBAL MEDICINE,SENT ME THE HERBAL MEDICINE THROUGH COURIER SERVICE, WHEN I RECEIVED THIS HERBAL MEDICINE USED IT FOR 2 WEEKS, AND 4 DAYS OF USAGE THE WARTS FELL OFF, MY MOTHER I NOW TOTALLY CURED AND MY MOTHER IS LIVING FREE AND HAPPY AGAIN. YOU CAN TALK TO DR VIA HIS MOBILE NUMBER OR WHATS APP HIM ON +2349038382931.ALL THANKS TO DOCTOR DR OLIHA
How can I explain this to the world that there is a man who can cure HERPES, I was diagnosed for the past 1 year I have being into HERPES since 1 year, so I decide to look for help in the internet then I found a post write about this great man called DR. Yakubu , people say good thing about him that this man have cured, a lot of people in the internet, him has power's to cure HSV1 AND HSV2 I don’t believe that there is a cure for Herpes Simplex Virus because though there is no cure for herpes that what I have in mind HERPES had no cure well , my HERPES is negative through the using of herbal cured of DR yakubu , I contacted this man for help because of what i see in the internet. if you need his cured just email him now on dr.yakubuherbalhealingclinic@gmail.com , thank you DR. i will never stop shearing you testimony DR. Yakubu . him Can as well CURE THE FOLLOWING DISEASE:-1, HIV/AIDS, 2, Diseases of the hear 3, Malignant tumors 4. Cardiovascular diseases 5. Diabetes mellifluous 6.Influenza and pneumonia 7.Alzheimer's disease 8. hsv1 - hsv2. If you need LOVE SPELL. E.T.C contact him dr.yakubuherbalhealingclinic@gmail.com or you whatsapp him on +2348057353647...
Dr.yakubu 하나님은 내 삶을 회복시켜 주신 것에 대한 축복을 계속할 것입니다. 나는 사람들에게 증거를 계속 나눌 것입니다.
ARE YOU AWARE THAT MODERN NATURAL HERBAL MEDICINES OF THIS GENERATION NOW PERMANENTLY CURE DRUG RESISTANT DISEASES LIKE; HSV/HERPES, CANCERS, HIV/AIDS, ERECTILE DISJUNCTION/ IMPOTENCY, DIABETES FOREVER WITHOUT A POSSIBLE COME BACK OR AFTER EFFECTS?
It wonderfully worked for me;
At first I was a bit skeptical about this Natural cure for herpes and other similar medicines. Discovering people with similar symptoms who are treated and cured by Dr Utu both on medias and in social medias on daily basis motivated me, so I contacted him for help!
At first, I was a bit curious about this possible cure, but! I don't want to be left out without giving it a trial, so I contacted him as well.
Some hours later he replied me, then he asked me some private questions, of which I honestly answered, I told him how I have lived and suffered with this disease and how much I will do anything to get rid of it. He assured me of total cure after taking his herbal medicines. It was even more easier than I expected. Also I never even imagined to get my parcels within five working days, but to my greatest surprise my parcels was brought to my doorstep by the end of the second day. I collected the parcel which I followed all the instructions as he had directed. Just as I was told "four weeks medication " my medicine finished in four weeks exactly. From week one of my medication I started noticing positive change in health. and in week two I could tell much more differences and I was so eager to even testify of life again in me.
I patiently continue medication till the last bottle which was then week four. I was the first person the next day in the clinic for lab test. Not even a particle of herpes was found in my system when I collected my result. Knowing I'm now herpes negative at this point I proceeded to inform my doctor, he doubted me, that day he gave me a month appointment to be closely monitored. It's my health so I waited more six Months and again i went for 'lab test' in a different clinical lab.
This time the result was still the same as the previous one. Also since this year I have been living my normal life and am still herpes free no symptoms and even till now no cold sore or outbreak. As a result of this herbal cure in my life and my family at large, I can boast of doctors today who through me, now uses African Traditional Roots and Herbs to TREAT AND CURE patients that are, CANCERS, HERPES, PARALYSIS, and HIV successfully today. Many are still ignorant of this I know.
Contact Dr Utu directly today on; "drutuherbalcure@gmail.com" to free yourself from emotional stress and become healthy again
I want to use this means to let the world know that all hope is not lost Getting pregnant after having tubes clamped and burned, I know IVF and Reversal could help but it way too cost, i couldn't afford it either and i so desire to add another baby to my family been trying for 5 years, not until i came across Priest Babaka, who cast a pregnancy/Fertility spell for me and i got pregnant.l hope that women out there who are going through the same fears and worries l went through in GETTING PREGNANT , will find your contact as i drop it here on this site, and solution will come to them as they contact you. Thank you and God bless you to reach him email via: babaka.wolf@gmail.com or Facebook at priest.babaka
Very impressive article! The blog is highly informative and has answered all my questions. To introduce about our company and the activities, Narwhal Data Partners is a database provider that helps you to boost your sales & grow your business through well-build ENT SPECIALIST EMAIL LISTS
I GOT RID OF HERPES WITHIN 12 DAYS
i am millian josh, from united state. i saw several comments on blog sites and Facebook page on how Dr OOSA cure people from herpes. after reading their article, i decided to ordered for Dr oosa medicine product which i received within 5 working days. i used the medicine for few days and my outbreak stop totally, and my herpes genital was gone completely. i went to hospital for test and the doctor confirmed i am herpes negative. i am sharing this story for herpes patient to know there is cure for herpes. here is DR OOSA email doctoroosaherbalhome@gmail.com or whatsapp +359878394269 his product is guarantee and its does not have any side effect
FINALLY FREE FROM HERPES VIRUS
I thought my life had nothing to offer anymore because life
became meaningless to me because I had Herpes virus, the
symptoms became very severe and bold and made my family
run from and abandoned me so they won't get infected. I gave
up everything, my hope, dreams,vision and job because the
doctor told me there's no cure. I consumed so many drugs but
they never cured me but hid the symptoms inside me making
it worse. I was doing some research online someday when I
came across testimonies of some people of how DR Ebhota
cured them from Herpes, I never believed at first and thought
it was a joke but later decided to contact him on the details
provided and when I messaged him we talked and he sent me
his herbal medicine and told me to go for a test after two
weeks. Within 7 days of medication the symptoms
disappeared and when I went for a test Lo and behold I was
NEGATIVE by the Doctor Who tested me earlier. Thank you DR
Ebhota because I forever owe you my life and I'll keep on
telling the world about you. If you are going through same
situation worry no more and contact DR Ebhota via
drebhotasolution@gmail. com or WhatsApp him via +2348089535482.
he also special on cureing 1. HIV/AIDS2. HERPES 3. CANCER 4.
ALS 5. HEPATITIS B 6.DIABETES 7. HUMAN PAPILOMA VIRUS DISEASE(HPV)8.
ALZHEIMER 9. LUPUS (Lupus Vulgaris or LupusErythematosus
I have been suffering from (HERPES) disease for the last four years and had constant pain, especially in my knees. During the first year, I had faith in God that I would be healed someday.This disease started to circulate all over my body and I have been taking treatment from my doctor, a few weeks ago I came on search on the internet if I could get any information concerning the prevention of this disease, on my search I saw a testimony of someone who has been healed from (Hepatitis B and Cancer) by this Man Dr. Silver and she also gave the email address of this man and advise we should contact him for any sickness that he would be of help, so I wrote to Dr. Silver telling him about my (HERPES Virus) he told me not to worry that I was going to be cured!! hmm i never believed it,, well after all the procedures and remedy given to me by this man few weeks later I started experiencing changes all over me as the Dr. assured me that I have cured, after some time i went to my doctor to confirmed if I have been finally healed behold it was TRUE, So friends my advice is if you have such sickness or any other at all you can email Dr. Silver (drsilverhealingtemple@gmail.com) sir I am indeed grateful for the help I will forever recommend you to my friends!!! with your lovely Email Address ( drsilverhealingtemple@gmail.com
I Want To Appreciate Dr.OYAGU for hs great deeds, I Was Diagnosed With type 2 Herpes Virus Last year,And Was Look For Solution To Be Cured Luckily I Saw Testimonies On How Dr.OYAGU Cure Herpes Virus I Decided To Contact Dr.OYAGU I Contacted Him He Prepared A Herbal Medicine Portion And Sent It To Me,I Started The Herbal Medicine For My Health.He Gave Me Step By Step Instructions On How To Apply It, When I Applied It As Instructed, I Was Cured Of This Deadly Herpes Within 2 weeks, I Am Now Herpes Negative.My Brother And Sister I No That There Are So Many People That Have There Same Herpes Virus Please contact Dr OYAGU To Help You Too,And Help Me To Thank Dr.OYAGU For Cure Me, I’m Cured By Dr. OYAGU Herbal Medicine,His Contact Email:oyaguspellcaster@gmail.com
Or Cell Whatsapp Number +2348101755322 thank you .....
I am so Happy to be writing this article in here, i am here to explore
blogs forum about the wonderful and most safe cure for HERPES SIMPLEX VIRUS
. I was positive to the deadly Virus called HERPES and i lost hope
completely because i was rejected even by my closet friends. i searched
online to know and inquire about cure for HERPES and i saw Dr Godwin
testimony online on how he was cured so many persons from Herpes Disease so
i decided to contact the great herbalist because i know that nature has the
power to heal everything. i contacted him to know how he can help me and he
told me never to worry that he will help me with the natural herbs from
God! After 2 days of contacting him, he told me that the cure is ready and
he will send it to me via FEDEX or DHL and it will get to me after 4 days!
i used the medicine as he instructed me (MORNING and EVENING) and i was
cured! its really like a dream but i'm so happy! That’s the reason i
decided to also add more comment of Him so that more people can be saved
just like me! and if you need his help ,contact his Email: ( Drgodwin
homeofsolution@gmail.com ) you can massage
him on whatsapp @ +2348054615060
I am very happy to inform the general public that I am finally cured from Herpes simplex virus recently with the use of herbal medicine, the powerful herbal medicine cured me completely and i was tested negative after usage, I am using this means to inform other's who have the virus that there is a cure for Herpes simplex 1&2 . It is absolutely true. I was cured by Dr Alli, only him I can recognize who cure Herpes perfectly well. I will advice you to contact this great doctor who God has send to put an end to the sorrowful and deadly disease. Contact him via Email Allispellhelp1@gmail.com or add him on WhatsApp +2348100772528
I Want To Appreciate Dr.OYAGU for hs great deeds, I Was Diagnosed With type 2 Herpes Virus Last year,And Was Look For Solution To Be Cured Luckily I Saw Testimonies On How Dr.OYAGU Cure Herpes Virus I Decided To Contact Dr.OYAGU I Contacted Him He Prepared A Herbal Medicine Portion And Sent It To Me,I Started The Herbal Medicine For My Health.He Gave Me Step By Step Instructions On How To Apply It, When I Applied It As Instructed, I Was Cured Of This Deadly Herpes Within 2 weeks, I Am Now Herpes Negative.My Brother And Sister I No That There Are So Many People That Have There Same Herpes Virus Please contact Dr OYAGU To Help You Too,And Help Me To Thank Dr.OYAGU For Cure Me, I’m Cured By Dr. OYAGU Herbal Medicine,His Contact Email:oyaguspellcaster@gmail.com
Or Cell Whatsapp Number +2348101755322 thank you .....
I am so Happy to be writing this article in here, i am here to explore blogs forum about the wonderful and most safe cure for HERPES SIMPLEX VIRUS.I was positive to the Virus called HERPES and i lost hope completely because i was rejected even by my closet friends. i searched online to know and inquire about cure for HERPES and i saw testimony about DR Ebhota online on how he cured so many persons from Herpes Disease so i decided to contact the great herbalist because i know that nature has the power to heal everything. i contacted him to know how he can help me and he told me never to worry that he will help me with the natural herbs from God! after 2 days of contacting him, he told me that the cure has been ready and he sent it to me via FEDEX or DHL and it got to me after 4 days! i used the medicine as he instructed me (MORNING and EVENING) and i was cured! its really like a dream but i'm so happy! that's the reason i decided to also add more comment of Him so that more people can be saved just like me! and if you need his help,contact his Email: (drebhotasoltion@gmail.com) You can contact him on WhatsApp +2348089535482 He also have the herb to cure difference cure for any sickness (1) HERPES,
(2) DIABETES,
(3) HIV&AIDS,
(4) URINARY TRACT INFECTION,
(5) HEPATITIS B,
(6) IMPOTENCE,
(7) BARENESS/INFERTILITY
(8) DIARRHEA
(9) ASTHMA..
I Want To Appreciate Dr.OYAGU for hs great deeds, I Was Diagnosed With type 2 Herpes Virus Last year,And Was Look For Solution To Be Cured Luckily I Saw Testimonies On How Dr.OYAGU Cure Herpes Virus I Decided To Contact Dr.OYAGU I Contacted Him He Prepared A Herbal Medicine Portion And Sent It To Me,I Started The Herbal Medicine For My Health.He Gave Me Step By Step Instructions On How To Apply It, When I Applied It As Instructed, I Was Cured Of This Deadly Herpes Within 2 weeks, I Am Now Herpes Negative.My Brother And Sister I No That There Are So Many People That Have There Same Herpes Virus Please contact Dr OYAGU To Help You Too,And Help Me To Thank Dr.OYAGU For Cure Me, I’m Cured By Dr. OYAGU Herbal Medicine,His Contact Email:oyaguspellcaster@gmail.com
Or Cell Whatsapp Number +2348101755322 thank you .....
i want to inform the public how i was cured of HERPES Simplex Virus by a Doctor called Dr.EBHOTA. i visited different hospital but they gave me list of drugs like Famvir, Zovirax, and Valtrex which is very expensive to treat the symptoms and never cured me. I was browsing through the Internet searching for remedy on HERPES and i saw comment of people talking about how Doctor EBHOTA cured them. I Was scared because i never believed in the Internet but i was convince to give him a try because i was having no hope of been cured of HERPES so i decided to contact him on his email, i searched his email on net and i saw a lot of people testifying about his goodness. when i contacted him he gave me hope and send a Herbal medicine to me that i took and it seriously worked for me, am a free person now without problem, my HERPES result came out negative. You can contact him on
his Email: drebhotasolution@gmail.com or whatsapp him on +2348089535482 and get all your problem solved.
1Sickness of any kind
2 Help to CURE Hepatitis B, HIV/AIDs CANCER and BIPOLAR
3 Divorce, Breakup problem and To Re-unit
4 Pregnancy problem
5 Financial problem and Job promotion
6 To get a good and rich life partner
7 To Lose your wath
8 to enlargement of pennis
9. CANCER
10. ALS (Lou Gehrig's disease)
11 Hepatitis B
12 chronic pancreatic
13 emphysema
14 COPD (chronic obstructive pulmonary disease)
HOW I GOT CURED OF HERPES DISEASEI'm here to testify about what DR. OSO did for me. I have been suffering from (HERPES) disease for the past 5 years and had constant pain,especially in my knees. During the first year,I had faith in God that i would be healed someday.This disease started circulating all over my body and i have been taking treatment from my doctor, few weeks ago i came across a testimony of one lady on the internet testifying about a Man called DR. OSO on how he cured her from herpes disease. And she also gave the email address of this man and advise anybody to contact him for help for any kind of sickness that he would be of help, so I emailed him telling him about my (HERPES) he told me not to worry that i was going to be cured!! Well i never believed it,, well after all the procedures and remedy given to me by this man few weeks later i started experiencing changes all over me as DR. OSO assured me that i will be cured,after some time i went to my doctor to confirmed if i have be finally healed behold it was TRUE,the test came out negative. So friends my advise is if you have such sickness or any other at all you can contact DR. OSO for help via email} drosohaberhome@gmail.com or WhatsApp+2348162084839.
here is the DR OSO website.
https://sites.google.com/view/drosohaberhome/
His blog page https://drosohaberhome.blogspot.com
you can also email me for more information about DR oso via smithmorgan2777@gmail.com ALL THANK TO DR OSO .
FINALLY FREE FROM HERPES VIRUS.
what a miracle i never believe there is cure because my doctor tested me herpes positive and she told me there is no cure, i’m very happy today that i’m having a free life without this herpes virus, i can remember some months ago when i was crying all through the night and day that i can’t get cured from this herpes, i found this herbal man called Dr sunny on internet when i was doing research on cure for shingle i contacted him to found out if i can get help from this herpes virus, i was so surprise when he told me that he have the herbs cure to it and he sent me the herbal in less down 5 days i was so happy when i get someone giving me hope that he can cured me i took the herbal for just 2 weeks, when i went for test after taking the herbal i found out that i am cured i was so happy and surprise, i want to use this opportunity to inform you that there is cured to herpes virus you can also contact him for his help as soon as possible so that you can get rid of this herpes once and for all you can reach him through this email: drsunnyna@gmail.com or whatsApp him on +2348077875210 You can also contact him on any disease and virus in this he all have the herbal cure to it.
1 HIV/AIDS
2 HERPES
3 CANCER
4 ALS
5 HEPATITIS
6 DIABETES
7 LOVE SPELL
8 INFECTIONS
9 HIGN BLOOD PRESSURE,.....
THANKS TO DR SUNNY FOE THE GOOD WORK IN LIFE YOU ARE TRULY A BLESS.....
FINALLY FREE FROM HERPES VIRUS
I thought my life had nothing to offer anymore because life
became meaningless to me because I had Herpes virus, the
symptoms became very severe and bold and made my family
run from and abandoned me so they won't get infected. I gave
up everything, my hope, dreams,vision and job because the
doctor told me there's no cure. I consumed so many drugs but
they never cured me but hid the symptoms inside me making
it worse. I was doing some research online someday when I
came across testimonies of some people of how DR Ebhota
cured them from Herpes, I never believed at first and thought
it was a joke but later decided to contact him on the details
provided and when I messaged him we talked and he sent me
his herbal medicine and told me to go for a test after two
weeks. Within 7 days of medication the symptoms
disappeared and when I went for a test Lo and behold I was
NEGATIVE by the Doctor Who tested me earlier. Thank you DR
Ebhota because I forever owe you my life and I'll keep on
telling the world about you. If you are going through same
situation worry no more and contact DR Ebhota via
drebhotasolution@gmail. com or WhatsApp him via +2348089535482.
he also special on cureing 1. HIV/AIDS2. HERPES 3. CANCER 4.
ALS 5. HEPATITIS B 6.DIABETES 7. HUMAN PAPILOMA VIRUS DISEASE(HPV)8.
ALZHEIMER 9. LUPUS (Lupus Vulgaris or LupusErythematosus
FINALLY FREE FROM HERPES VIRUS
I thought my life had nothing to offer anymore because life
became meaningless to me because I had Herpes virus, the
symptoms became very severe and bold and made my family
run from and abandoned me so they won't get infected. I gave
up everything, my hope, dreams,vision and job because the
doctor told me there's no cure. I consumed so many drugs but
they never cured me but hid the symptoms inside me making
it worse. I was doing some research online someday when I
came across testimonies of some people of how DR Ebhota
cured them from Herpes, I never believed at first and thought
it was a joke but later decided to contact him on the details
provided and when I messaged him we talked and he sent me
his herbal medicine and told me to go for a test after two
weeks. Within 7 days of medication the symptoms
disappeared and when I went for a test Lo and behold I was
NEGATIVE by the Doctor Who tested me earlier. Thank you DR
Ebhota because I forever owe you my life and I'll keep on
telling the world about you. If you are going through same
situation worry no more and contact DR Ebhota via
drebhotasolution@gmail. com or WhatsApp him via +2348089535482.
he also special on cureing 1. HIV/AIDS2. HERPES 3. CANCER 4.
ALS 5. HEPATITIS B 6.DIABETES 7. HUMAN PAPILOMA VIRUS DISEASE(HPV)8.
ALZHEIMER 9. LUPUS (Lupus Vulgaris or LupusErythematosus
TESTIMONY ON HOW I CURED MY CANCER! . All thanks too @dr_adazal6Hey! I can,t believe this. A great testimony that i must share to all cancer patient in the world i never believed that their could be any complete cure for lung cancer or any cancer,i saw people testimony on blog sites of how @dr_adazal6 Simpson cannabis oil brought them back to life again. i had to try it too and you can’t believe that in just few weeks i started using it all my pains stop gradually and i had to leave without the drugs the doctor gave to me. Right now i can tell you that for months now i have not had any pain, and i have just went for text last week and the doctor confirmed that there is no trace of any cancer system. Glory be to God for leading me to this genuine Man Dr adazal Simpson. I am so happy as i am sharing this testimony. My advice to you all who thinks that their is no cure for cancer that is Not true, just contact him and get cannabis oil from dr.adazal Simpson to cure your cancer and you will be free and free for ever, Try it and you will not regret it because it truly works. One thing i have come to realize is that you never know how true it is until you try. There is no harm in trying. Remember, delay in treatment leads to death. Here is his com Contact him and be free from cancer! I wish you a quick recovery WhatsApp number+. +2348073688335 or email via dr.adazalherbalcure@gmail.com
I am really happy that i have been cured from (HERPES SIMPLEX VIRUS) with the herbal medicine of Dr OSAGIE , i have been suffering from this disease for the past 3 years and 4 mouth without solution until i came across the email of this doctor who have cure so many people with his herbal medicine, i also choose to give him a chance to help me and my husband, he told me what to do and i kindly did it, and he gave us his herbal medicine and direct me on how to use it, i also follow his instructions for use and he ask us to go for a check up after 1 week and 5days which i did, to my greatest surprise our result came out as negative, we are really happy that there is someone like this doctor who is ready to help anytime any day. To all the readers and viewers that is doubting this testimony stop doubting it and contact this doctor if you really have one and see if he will not actually help you. i am not a stupid woman that i will come out to the public and start saying what someone have not done for me and i know that there are some people out there who are really suffering and hurting their family just because of these diseases so you can to mail him on drosagiesolutiontemple@gmail.com OR
DROSAGIESOULTIONTEMPLE@YAHOO.COM or WHATSAPP +2347030465649 follow him on his Instagram account @dr_osagie_88 he also told me that he has cure for these diseases listed below .
HERPES SIMPLEX VIRUS.
.DIABETES .
CANCER
.HEPATITIS
.HIV/AIDS
Thank you for your time
I am from New York. I was in trouble when doctor told me that I have been
diagnosed tinnitus ringing ears with … I though about my Family, I know my Family will
face a serious problem when I’m gone, I lost hope and I wept all day, but one
day I was surfing the Internet I found Dr. Emmanuel contact number. I called him
and he guided me. I asked him for solutions and he started the remedies for my
health. Thank God, now everything is fine, I’m cured by Dr. Emmanuel herbal
medicine, I’m very thankful to Dr. Emmanuel and very happy with my hubby and
family. email him on traditionalherbalhealingcentre@gmail.com OR contact his whatsapp number:
+2348140033827
DOCTOR EMMANUEL CAN AS WELL CURE THE FOLLOWING DISEASE:-
1. HIV/AIDS
2. HERPES
3. CANCER
4. ALS
5. DIABETES
6. HEPATITIS
I’m from USA am here to give my testimony about Dr Voke who helped me cure my HERPES (HSV), i want to inform the public how i was cured from (HERPES SIMPLEX VIRUS), i visited different hospital but they gave me list of drugs like Famvir, Zovirax, and Valtrex which is very expensive to treat the symptoms and never cured me. Three months ago a friend suggested that I try herbal medicine; from a very powerful herbal doctor called (doctorvoke@gmail.com) I looked up his blog on the internet site and indeed he have had immense success with his product. There were lot of persons posting their testimony about how he cured them. when i contacted him he gave me hope and send a Herbal medicine to me that i took and it seriously worked for me, my HERPES result just came out negative. (doctorvoke@gmail.com)
I’m from USA am here to give my testimony about Dr Voke who helped me cure my HERPES (HSV), i want to inform the public how i was cured from (HERPES SIMPLEX VIRUS), i visited different hospital but they gave me list of drugs like Famvir, Zovirax, and Valtrex which is very expensive to treat the symptoms and never cured me. Three months ago a friend suggested that I try herbal medicine; from a very powerful herbal doctor called (doctorvoke@gmail.com) I looked up his blog on the internet site and indeed he have had immense success with his product. There were lot of persons posting their testimony about how he cured them. when i contacted him he gave me hope and send a Herbal medicine to me that i took and it seriously worked for me, my HERPES result just came out negative. (doctorvoke@gmail.com)
I am from New York. I was in trouble when doctor told me that I have been
diagnosed tinnitus ringing ears with … I though about my Family, I know my Family will
face a serious problem when I’m gone, I lost hope and I wept all day, but one
day I was surfing the Internet I found Dr. Emmanuel contact number. I called him
and he guided me. I asked him for solutions and he started the remedies for my
health. Thank God, now everything is fine, I’m cured by Dr. Emmanuel herbal
medicine, I’m very thankful to Dr. Emmanuel and very happy with my hubby and
family. email him on traditionalherbalhealingcentre@gmail.com OR contact his whatsapp number:
+2348140033827
DOCTOR EMMANUEL CAN AS WELL CURE THE FOLLOWING DISEASE:-
1. HIV/AIDS
2. HERPES
3. CANCER
4. ALS
5. DIABETES
6. HEPATITIS
Is any one here suffering from any kind of STD or STI ? , Now this is to everyone out there with different health challenges, as I know there are still a lot of people suffering from different health issues and are therefore looking for solution. I bring you Good news. There is a man called Dr. Tokubo a herbal practitioner who helped cure me from Genital herpes, this i had suffered from for the past 2years and have spent so much money trying to survive from it. I got my healing by taking the herbal medicine he sent to me to drink for about 9days . 3days after completion of the dosage, I went for a medical checkup and I was tested Genital Herpes NEGATIVE. I'm sharing this so that other people can know of this great healer called Dr Tokubo because I got to know him through a friend he cured from HIV. I was made to understand that he can cure several other deadly diseases and infections. Don't die in ignorance and don't let that illness take your life. Contact Dr. Tokubo through: drtokubotemple@gmail.com You can also call/whatsapp him on:+2349037990322 Thank you dr tokubo. Be kind enough to share your testimonies as you received your cure.he is good too to cure all type of disease and virus.1 HIV cure
2 cancer
3 diabetes
4 hepatitis
5 herpes
6 HIV.
You can contact him if you are having any disease or infection problem...
If you need ( cure to Herpes virus ) and treatment to all illness___________________!!!!!!!!!!!!!!!!!!
-[HPV]
-[DIABETES]
-[WEAK ERECTION]
-[[WHOOPING COUGH]]
–[[HEPATITIS A,B AND C]]
-[[COLD SORE]]
-[[LOWER RESPIRATORY INFECTION]]
-[[LOW SPERM COUNT]]
-[[STAPHYLOCOCCUS AUREUS]]
-[[STROKE]]
-[[IMPOTENCE]]
-[[PILE]]
-[[HYPERTENSION]]
-[[MENOPAUSE DISEASE]]
-[[ASTHMA]]
-[[CANCER]]
-[[SHINGLES]]
-[[FIBROID]]
-[[TINNITUS]]
-[[YEAST INFECTION]]
-[[BARENESS/INFERTILITY]]…
Please contact:
Email Doctorvoke@yahoo. com
Sure Treatment!!
Glad i was cured from herpes…
Good day to all viewer online am so happy sharing this great testimony on how i was checking for solution in the internet then miraculously i came Across Dr.Aire the powerful herbalist that Cure Numerous individuals Herpes Simplex Virus,so I contacted him base on the testimonies I?m seeing about him on the internet, I was cured too by him, kindly contact him actoday through his email he can help you email ; drairehome@gmail.com OR WHATSAPP +2347036740271
Dr. Riaria cured my herpes virus that have been in my body since two years, ever since then my life has been incomplete, I have used so many drugs that was prescribed to me by doctors, but it didn't cure my herpes virus, i was checking for solution on the internet then I miraculously came across Dr. Riaria the powerful herbalist that can cure herpes infection, then I contacted him through his email, I explained everything to him and he prepared a herbal medicine and sent it to me through FedEx, which I took for 14 days with the instruction he gave me, and when I did a test in the hospital my result came out negative it was the happiest day of my life that am cure from HSV 2, are you also suffering from same virus or another diseases you can simply contact him via email: drriaria@gmail.com you can also call or WhatsApp him on: +2349134987375.
nice post..Best Gynecologist In Tirunelveli
best doctors in Tirunelveli'
Hello viewers I am glad to have met with the powerful herbal healer called
Dr voodoo who use his herbs to cure my HIV disease I suffered from 15years,
but now I am a happy woman and i am free from this sickness that has been
problem to my living, after using Dr voodoo herbal medicine within 1week i
was diagnose negative, I will recommend Dr voodoo to everyone reading this
article because this herbal healer is capable to heal anything, the
scientist said has no cure, Email him : voodoospelltemple66@gmail.com or
add Dr voodoo on whatsApp: +234814012071
I started on COPD Herbal treatment from Ultimate Life Clinic, the treatment worked incredibly for my lungs condition. I used the herbal treatment for almost 4 months, it reversed my COPD. My severe shortness of breath, dry cough, chest tightness gradually disappeared. Reach Ultimate Life Clinic via their website at www.ultimatelifeclinic.com I can breath much better and It feels comfortable!
DO YOU NEED A PERSONAL/BUSINESS/INVESTMENT LOAN? CONTACT US TODAY VIA WhatsApp +19292227023 Email drbenjaminfinance@gmail.com
HELLO
Loan Offer Alert For Everyone! Are you financially down and you need an urgent credit/financial assistance? Or are you in need of a loan to start-up/increase your business or buy your dream house. GET YOUR INSTANT LOAN APPROVAL 100% GUARANTEED TODAY NO MATTER YOUR CREDIT SCORE. WhatsApp:+19292227023 Email: drbenjaminfinance@gmail.com
I have been suffering from (HERPES) disease for the last four years and had constant pain, especially in my knees. During the first year, I had faith in God that I would be healed someday.This disease started to circulate all over my body and I have been taking treatment from my doctor, a few weeks ago I came on search on the internet if I could get any information concerning the prevention of this disease, on my search I saw a testimony of someone who has been healed from (Hepatitis B and Cancer) by this Man Dr. Ehimare and she also gave the email address of this man and advise we should contact him for any sickness that he would be of help, so I wrote to Dr. Ehimare telling him about my (HERPES Virus) he told me not to worry that I was going to be cured!! hmm i never believed it,, well after all the procedures and remedy given to me by this man few weeks later I started experiencing changes all over me as the Dr. assured me that I have cured, after some time i went to my doctor to confirmed if I have been finally healed behold it was TRUE, So friends my advice is if you have such sickness or any other at all you can email Dr. Ehimare (drehimare3@gmail.com) or via whatsapp+ 1 (267) 691-1087 sir I am indeed grateful for the help I will forever recommend you to my friends!!!
There is a great herbal man called Dr voodoo who can cure Hepatitis B virus and other deadly diseases with the use of natural herbs to cure Hepatitis B virus problems. He is from Africa and he is a great doctor and he can also cure you as well if you are have the problem And other deadly disease and here is email address voodoospelltemple66@gmail.com or Whatsapp +2348140120719 HERPES CURE,CANCER CURE,HIV/AIDS CURE,HPV CURE
Ear Wax Removal clinic at Sutton Coldfield/ Tamworth/ Staffordshire and surrounding areas. We use endoscopic microsuction for safe removal.
<a href=" https://earwaxspecialist.co.uk/ear-wax-removal-sutton-coldfield/”> ear wax removal tamworth </a>
Ear Wax Removal clinic at Sutton Coldfield/ Tamworth/ Staffordshire and surrounding areas. We use endoscopic microsuction for safe removal. https://earwaxspecialist.co.uk/ear-wax-removal-sutton-coldfield
Look no further than Earwego LTD if your ears are blocked with ear wax and you're looking for the best earwax cleaning clinic to gClear Earwax Blockage at Home in Nottinham.  
Eliminate Herpes simplex virus (HSV) forever..through herbal means…💯💯💯💯💯
This herbal Doctor has a new development on herpes virus,
certainly the best online…
Thank you!! for saving my life 🙏🏽🙏🏽🙏🏽
Email:Robin son buc kler (( @yahoo .com))…………
I was diagnosed with Bronchiectasis four years ago. For over two years, I relied on prescription medications and therapies, but unfortunately, the symptoms continued to worsen. My breathing became more laboured, and I experienced increasing fatigue and shortness of breath with even minimal activity. Last year, out of desperation and hope, I decided to try an herbal treatment program from NaturePath Herbal Clinic. Honestly, I was skeptical at first, but within a few months of starting the treatment, I began to notice real changes. My breathing became easier, the tightness in my chest eased, and I felt more energetic and capable in my daily life. Incredibly, I also regained much of my stamina and confidence. It’s been a life-changing experience I feel more like myself again, better than I’ve felt in years. If you or a loved one is struggling with Bronchiectasis, I truly recommend looking into their natural approach. You can visit their website at www.naturepathherbalclinic.com
info@naturepathherbalclinic.com
Post a Comment