- The term dyspnea implies an unpleasant sensation of shortness of breath that is out of proportion to the ventilatory needs expected for a given level of work.
- Dyspnea is commonly seen in association with the diseases of pulmonary and cardiovascular systems
- Orthopnea refers to dyspnea in the supine position that is relieved by assuming an upright posture and is typically seen in left ventricular failure.
- Trepopnea is dyspnea that occurs when the patient is in the right or left lateral decubitus position.
- Dyspnea in the upright position that is relieved by resuming the supine posture is called platypnea, from platys, meaning recumbent, and pnoe, meaning breath. It may be associated with a decrease in arterial oxygen saturation when the patient changes from the supine to the upright position, called orthodeoxia, from orthos, meaning upright, and deoxia, meaning desaturation.
Platypnea-orthodeoxia is a rare syndrome that is caused by a diverse set of cardiac, pulmonary, and hepatic diseases. The predominant symptom, dyspnea induced by upright posture, can be debilitating and difficult to discern without thorough evaluation of the patient's pattern of dyspnea. The cause revolves mostly around an intracardiac right-to-left shunt or intrapulmonary shunts
Clinical states associated with the platypnea-orthodeoxia syndrome:
- Intracardiac right-to-left shunts (patent foramen ovale or atrial septal defect)
- After pulmonary resection (eg, pneumonectomy, lobectomy)
- Associated cardiac abnormality (eg, aortic aneurysm, pericardial effusion)
- Associated skeletal deformity (kyphoscoliosis)
- Intrapulmonary right-to-left shunts
- congenital: Osler-Weber-Rendu syndrome(characterized by pulmonary AV malformations-Pulmonary AVMs may cause enough right-to-left shunting)
- acquired: vascular dilations in Hepatopulmonary syndrome
- Hepatopulmonary syndrome
- Pulmonary diseases
- Chronic obstructive pulmonary disease
- Pulmonary embolism
- Upper airway tumor
- Acute respiratory distress syndrome
- Autonomic neuropathy
Cardiac Causes
- The most common cause of platypnea-orthodeoxia is an intracardiac right-to-left shunt, often present as patent foramen ovale (PFO).
- The condition becomes manifest as a consequence of anatomic changes after surgery (pneumonectomy or lobectomy) or development of kyphoscoliosis, aortic aneurysm,or aortic elongation.
- Other conditions reported to produce platypnea in the presence of PFO include pericardial effusion,constrictive pericarditis, eosinophilic endomyo-cardial disease,idiopathic hemidiaphragm paralysis, compression of right heart by a large hydatid cyst of liver, and blunt chest wall trauma.
- Typically, patients have normal pulmonary artery pressures.
Mechanisms of Platypnea-Orthodeoxia:
- Two conditions must coexist to cause platypnea-orthodeoxia:
- an anatomical component in the form of an interatrial communication and
- a functional component that produces a deformity in the atrial septum and results in a redirection of shunt flow with the assumption of an upright posture.
- The former may be an atrial septal defect, a patent foramen ovale, or a fenestrated atrial septal aneurysm.
- The latter may be cardiac, such as pericardial effusion or constrictive pericarditis; pulmonary, such as emphysema, arteriovenous malformation, pneumonectomy, or amiodarone toxicity; abdominal, such as cirrhosis of the liver or ileus; or vascular, such as aortic aneurysm or elongation
Under normal conditions an interatrial communication allows blood to shunt from left to right due to a higher pressure in left atrium than right atrium and a greater compliance of the right ventricle than the left ventricle.
Right-to-left interatrial shunting is usually associated with spontaneous or induced pulmonary hypertension and, therefore, in the absence of a right-to-left pressure gradient, what is the mechanism for a right-to-left shunt?
Or put in another way, what causes water to flow uphill?
A persistent Eustachian valve can cause interatrial right-to-left shunting with a normal right atrial pressure. Platypnea-orthodeoxia could be explained on the basis of positional modification of abnormal shunting.
Standing upright could stretch the interatrial communication, be it a patent foramen ovale, an atrial septal defect, or a fenestrated atrial septal aneurysm, thus allowing more streaming of venous blood from inferior vena cava through the defect, whether or not a persistent Eustachian valve coexists.
This redirection of flow caused by an anatomic distortion of the right atrium or the atrial septum also might occur from a loculated pericardial effusion, an aortic aneurysm, or aortic elongation
Pulmonary Causes
- In the normal lung, blood flow is greater at the bases compared with the apical regions because of the effects of gravity, whereas the alveolar pressure remains constant throughout the lung.
- In various lung diseases, alveolar pressures become substantially elevated as a result of alterations of ventilatory mechanics (diffuse Zone I phenomenon).
- It is proposed that the assumption of an upright posture would increase this tendency, especially in the apical portions of the lung, because of a drop in pulmonary artery pressure, leading to pulmonary capillary compression.
- The combination of these two phenomena could lead to the cessation of blood flow, resulting in a respiratory dead space.
- The increased dead space causes dyspnea and hyperventilation, which augments air trapping, which further increases the alveolar pressure, initiating a vicious cycle.
Hepatic Causes
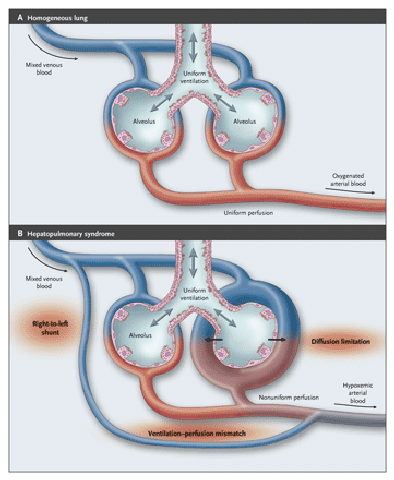
The hepatopulmonary syndrome (HPS) is a triad of liver disease, increased alveolar-arterial oxygen gradient, and intrapulmonary vascular dilatations.
set of four diagnostic criteria for the hepatopulmonary syndrome:
- Presence of chronic hepatic disease (alcoholic, post-necrotic, or primary biliary cirrhosis or active chronic hepatitis). Severe liver dysfunction may not be mandatory.
- Absence of intrinsic cardiopulmonary disease, with normal chest radiograph or with nodular basal shadowing.
- Pulmonary gas exchange abnormalities. An increased alveolar-arterial oxygen gradient (>/= 20 mm Hg) with or without hypoxemia.
- The extrapulmonary appearance of IV radiolabeled microspheres or a positive contrast-enhanced echo-cardiogram, suggesting intrapulmonary vascular abnormalities.
- The unique striking pathological feature of hepatopulmonary syndrome is gross dilatation of the pulmonary precapillary and capillary vessels (to 15 to 100 µm in diameter when the patient is at rest), coupled with an absolute increase in the number of dilated vessels visualized by means of injection at autopsy.
In addition, a few pleural and pulmonary arteriovenous communications (shunts) and portopulmonary venous anastomoses can be seen.
The prerequisite of pulmonary vascular dilatation facilitates the passage of mixed venous blood either rapidly or even directly, through intrapulmonary shunt, into the pulmonary veins.Because of gravity, shifting of blood to the dilated precapillary beds of the lung bases results in an increased hypoxemic dyspnea when the patient is in the upright position.
Ventilation–perfusion mismatch emerges as the predominant mechanism.
4 comments:
Here is a great herbal doctor who cured me of Hepatitis B. his name is Dr. Imoloa. I suffered Hepatitis B for 11 years, I was very weak with pains all over my body my stomach was swollen and I could hardly eat. And one day my brother came with a herbal medicine from doctor Imoloa and asked me to drink and I drank hence there was no hope, and behold after 2 week of taking the medicine, I started feeling relief, my swollen stomach started shrinking down and the pains was gone. I became normal after the completion of the medication, I went to the hospital and I was tested negative which means I’m cured. He can also cure the following diseases with his herbal medicine...lupus, hay fever, measles, dry cough, diabetics hepatitis A.B.C, mouth ulcer, mouth cancer, bile salt disease, fol ate deficinecy, diarrhoea, liver/kidney inflammatory, eye cancer, skin cancer disease, malaria, chronic kidney disease, high blood pressure, food poisoning, parkinson disease, bowel cancer, bone cancer, brain tumours, asthma, arthritis, epilepsy, cystic fibrosis, lyme disease, muscle aches, fatigue, muscle aches, shortness of breath, alzhemer's disease, acute myeloid leukaemia, acute pancreatitis, chronic inflammatory joint disease, Addison's disease back acne, breast cancer, allergic bronchitis, Celia disease, bulimia, congenital heart disease, cirrhosis, constipation, fungal nail infection, fabromyalgia, (love spell) and many more. he is a great herbalist man. Contact him on email; drimolaherbalmademedicine@gmail.com. You can also reach him on whatssap- +2347081986098.
Dear Maria Rose, the so called Dr. Imoloa is a bunch of bullshit. Google his name and comments (like yours) from a bunch of blog sites pop up. If what you say is true he should have won the noble prize in medicine, but alas, its all fake bullshit.
Sincerely,
Western Medicine
I started on COPD Herbal treatment from Ultimate Health Home, the treatment worked incredibly for my lungs condition. I used the herbal treatment for almost 4 months, it reversed my COPD. My severe shortness of breath, dry cough, chest tightness gradually disappeared. Reach Ultimate Health Home via their website www.ultimatelifeclinic.com . I can breath much better and It feels comfortable!
Thank You and I have a super provide: Who Repairs House Siding best renovations to increase home value
Post a Comment